
Table of Contents
-
Trends at the Heart of Healthcare’s Transformation
Trend 1 : Emergence of New Tech-enabled Business Models
Transformation of Healthcare, Intensifying Competition
Trend 2 : Transformation of Healthcare Systems Picks Pace
The tectonics are Shifting; Getting at the Core of Change
Trend 3 : A Fundamental Shift Towards Outcome and Value Oriented Healthcare
How the Focus is Shifting Towards Wellness
Trend 4 : Meteoric Rise of Telemedicine and Telehealth - Is the Trend Here to Stay?
Paradigm Shifts, Technology, Regulations, Medical Errors and More.
Trend 5 : Patient Experience Gets the Center Stage
Pandemic has put Patients at the Center, and Digital is making their voice count
Trend 6 : Digital Transformation in Healthcare Picking up Heat
Emergence of new digital entities
DX in the unique context of Healthcare
Trend 7 : Hyper-growth of Comprehensive IT Platforms and Applications
Designing Perfect mHealth Applications
Factors influencing success of mHealth apps and more.
Trend 8 : Remote Monitoring and Patient Engagement Become Integral
Apart from Synchronous Telemedicine the other areas of Telehealth are getting renewed focus
Trend 9 : Institutional Investments Silently Shaping Healthcare’s Evolution
Trend 10 : Rise of VR with New Use Cases
Trend 11 : Ascent of Big Data and AI
Trend 12 : Increasing Awareness towards Data Privacy and Cybersecurity
The Esteemed Collaborators:
We thank each of the following experts who were interviewed for this paper. Our heart-felt gratitude towards them for giving their precious time and invaluable insights that have added immense value to the paper.
Jay is known to many as the Father of Telemedicine, he developed the first statewide telemedicine system. He is the CEO of The Global Telemedicine Group, Professor of Medicine (Adjunct) at Johns Hopkins School of Medicine and a Founding Board Member and President Emeritus of the American Telemedicine Association.
He spoke to us on the Nitty-Gritty and future of Telemedicine.
Christine is the founder and Managing Director of Digi-Bridges, she started to help unleash the potential of using Digital Strategies in advancing healthcare.
Christine is also a HealthTech researcher at ARU in Cambridge and teaches Digital Marketing and Communications at the University of Applied Sciences Northwest Switzerland.
Christine spoke to us on the performance of a mHealth tool or applications and on crafting strategies to ensure wider adoption and success. Her research disambiguates the factors that influence technological adoption in healthcare.
Helen is the founder Tigon Advisory, a CXO-as-a-Service growth accelerator to multiply growth opportunities for organizations.
Helen is a Global Top 20 thought leader in 10 categories, including digital transformation, AI, cloud computing, Cybersecurity, IoT and Marketing.
Being a leading Digital Transformation expert and influencer, Helen spoke with Techment on the subject of DX in the unique context of Healthcare, emerging role of IT platforms, challenges, and patient experience.
Dr. Vikram is the founder and editor of Healthcare India, a think tank that is passionate about building futuristic models for healthcare in India.
Dr. Vikram serves on various industry committees on healthcare and has published papers on a wide range of topics like Patient Experience, Blockchain, and Public Health. His area of expertise lies in devising healthcare strategy, go to market strategy, customer acquisition, digital health, and healthcare public policy.
Dr. Vikram spoke to us on the fundamental shift in healthcare and DX.
Executive Summary
The traditional health care model is dead! And there is no going back. Some organizations at the current crossroad will use data, and digital technologies to serve patients in new, unique and innovative ways, others will grudgingly grapple with change to see an inevitable decline.
Technology can add an astonishing amount of value in terms of cost and quality - over US$ 500 bn, and cut down the expenditure growth by 30%; you can further add the value of innovation, and yes, the potential of health IT is boundless!
Digital technology is also our only hope of solving the Iron Triangle of - Access, Affordability, and Effectiveness. In the age of Google, Apple and Amazon, patients have begun to seek healthcare in accessible, engaging, and outcome driven formats.
Tech and healthcare could become bedfellows in unimaginable ways.
We are looking at the birth of new ecosystems that bring together diverse stakeholders, and deliver care to the farthest. Telemedicine, diagnostic devices, IMoTs, wearable devices have shown a shimmer of possibilities. For the first time we are seeing a focus on patient experience, and in delivering care in the best possible way. However, the question remains – are we going to regress back, will regulations thwart innovation, will data security, privacy concerns and cyber attacks deter us?
We spoke to the world’s leading healthcare experts, physicians, researchers, and influencers from around the globe to understand the essence of change that is happening, and how companies can best strategize to deliver the most value. Change will not be easy as the challenges of legacy systems, practices, apprehensions and conservative regulations are formidable. We need collective will to resurrect healthcare!
Introduction
The virus has illustrated just how vulnerable the present healthcare system is and how little ech-driven innovation has reached it. As we grapple with this global existential crisis, the tech community has to assume a new level of responsibility and proactively tackle the challenge at hand.
The world is seeing a patient centric transition from “sick care” to “health assurance” that would eventually become the core motive of people to subscribe to healthcare services. Digital technologies will play a vital role in this transition by connecting and managing fragmented healthcare systems.
The use cases of digital technologies are rapidly expanding; VR/AR, MIoT, AI/ML, automation and digital transformation hold the key to radically new approaches to healthcare.
The US for instance is facing its worst drug crisis, and a consequent economic burden of $78.5 billion a year and technology software platforms and VR - are better equipped in treating than pharmaceuticals.
In reality, very few areas in healthcare have seen costs decrease to any real degree2. Due to large costs involving the treatment of illnesses, the healthcare industry has evolved into an insurance-based industry. Pandemic has exposed other issues with the system necessitating digital to become an integral part of healthcare as insurance is today.
In this paper we have discussed competition between new entrants and incumbents and elaborated how digital health innovations contribute to the changing role of patients.
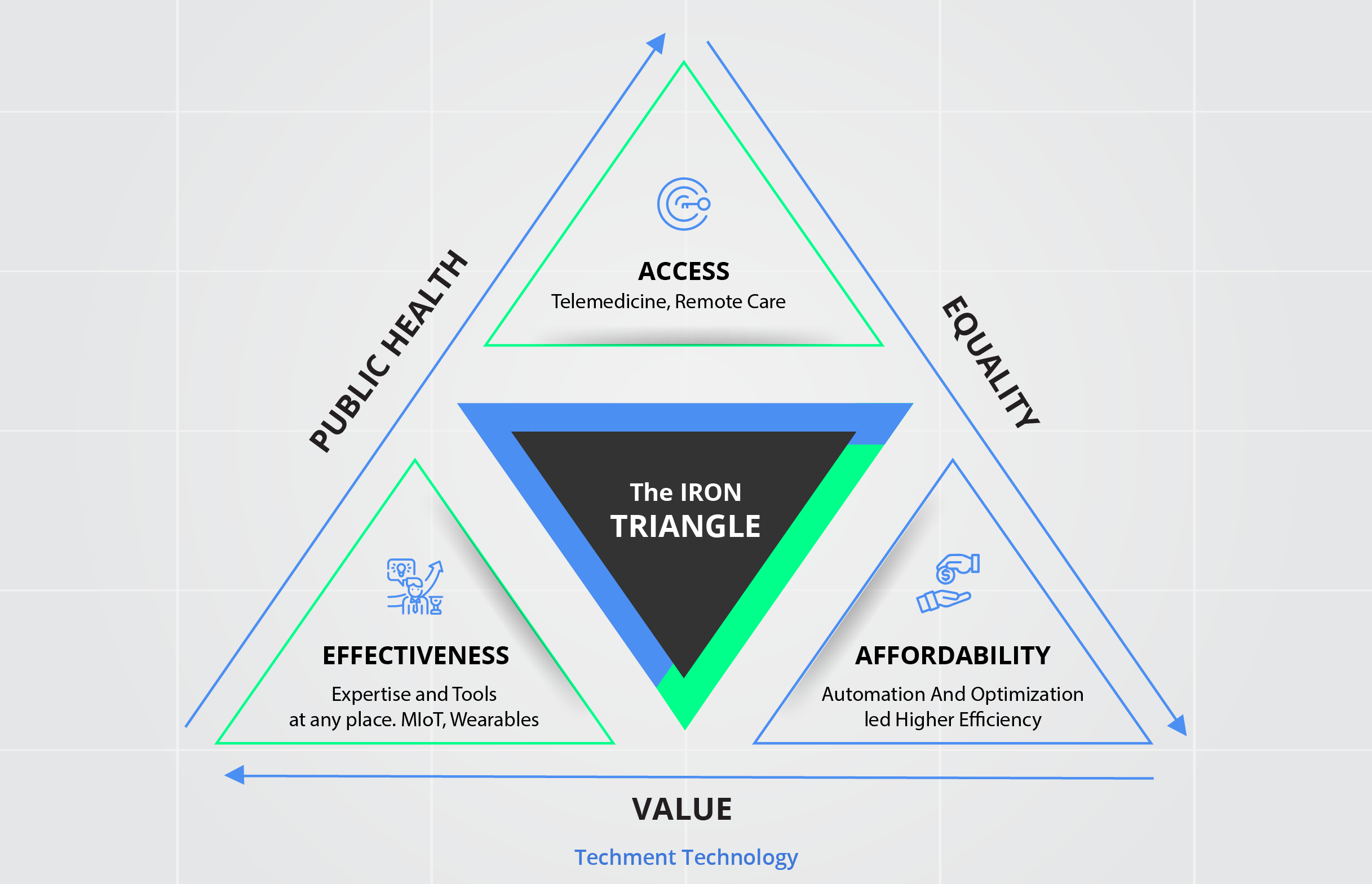
Technology Solving the Iron Triangle of Healthcare Sector
Digital can potentially solve the problem of the “Iron Triangle’’ - It involves three interlocking factors which are, namely, Access, Affordability, and Effectiveness. While trying to improve one factor the other usually falls behind. Digital helps optimize old methods, slashes cost and innovates for better care, while also increasing the accessibility of the services.
Rising Health Expenditure & Need for Technology
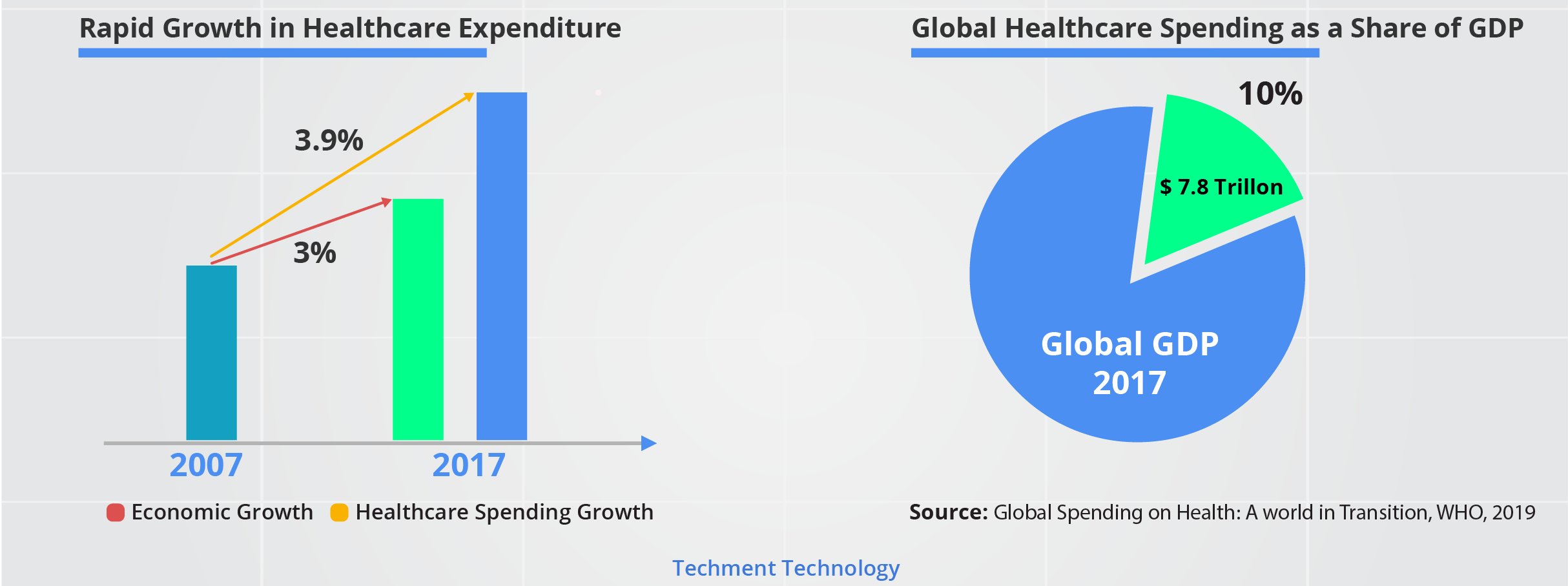
Rising Healthcare Expenditure
Global spending on health continues to rise; it was US$ 7.8 trillion in 2017, or about 10% of GDP.
The health sector continues to expand faster than the economy. Between 2000 and 2017, global health spending in real terms grew by 3.9% a year while the economy grew 3.0% a year (WHO).
3. Segments of Virtual Care
Virtual care has become a giant with expanding Tech capabilities. There are the major areas where hospitals and clinics and other players need to invest as they touch every aspect of care delivery.
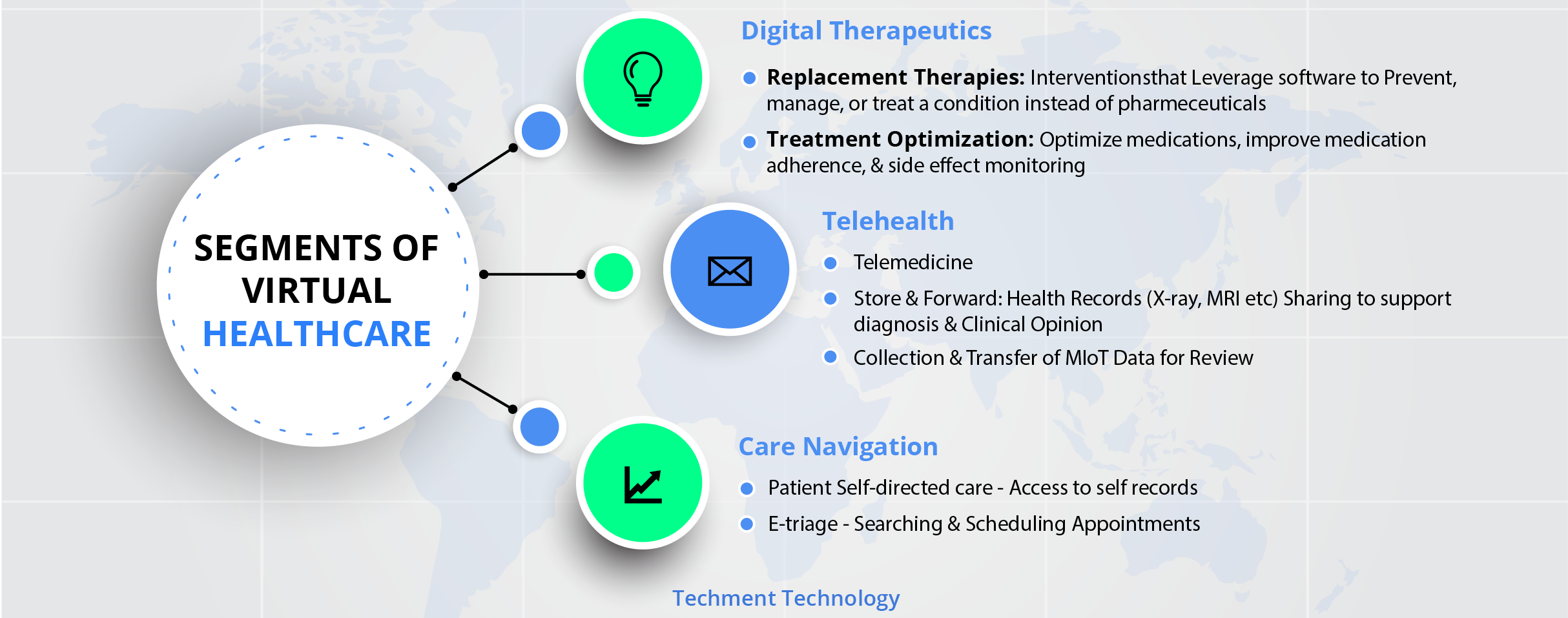
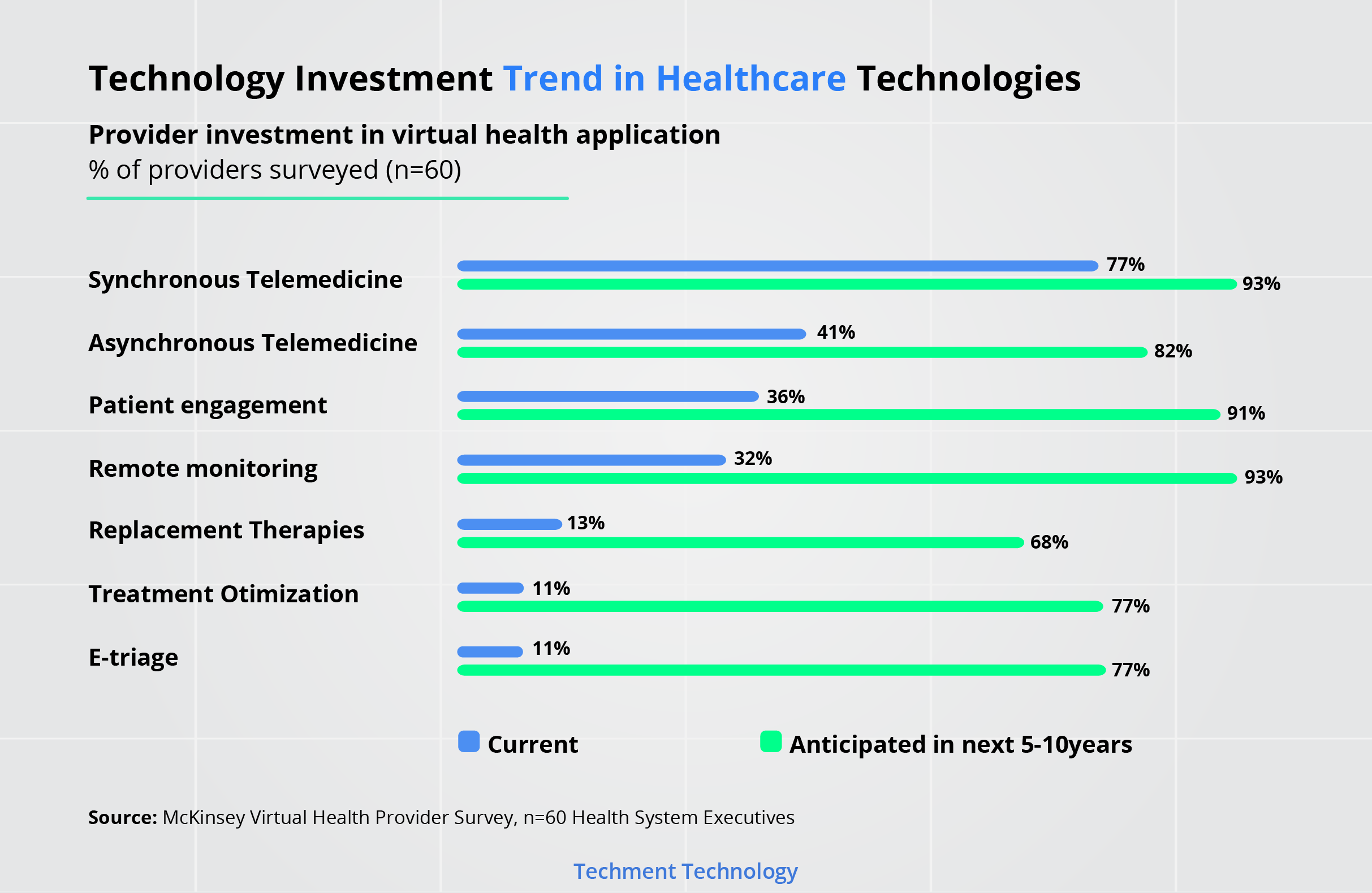
Prior to COVID-19, a 2019 McKinsey survey3 health system leaders revealed that virtual health adoption was highly concentrated in synchronous telemedicine, with limited investment in the full capabilities of virtual healthcare technologies. Leaders indicated that - Remote Monitoring - as a major area for future investment.
The future areas of investment as revealed by:
-
Asynchronous Telemedicine
-
Patient Engagement
-
Remote monitoring
-
Replacement therapies
-
Treatment Optimization
-
E-triage
4. ‘5’ Models of Care Delivery
These delivery models require engagement of various elements of healthcare delivery systems to build omnichannel care models.
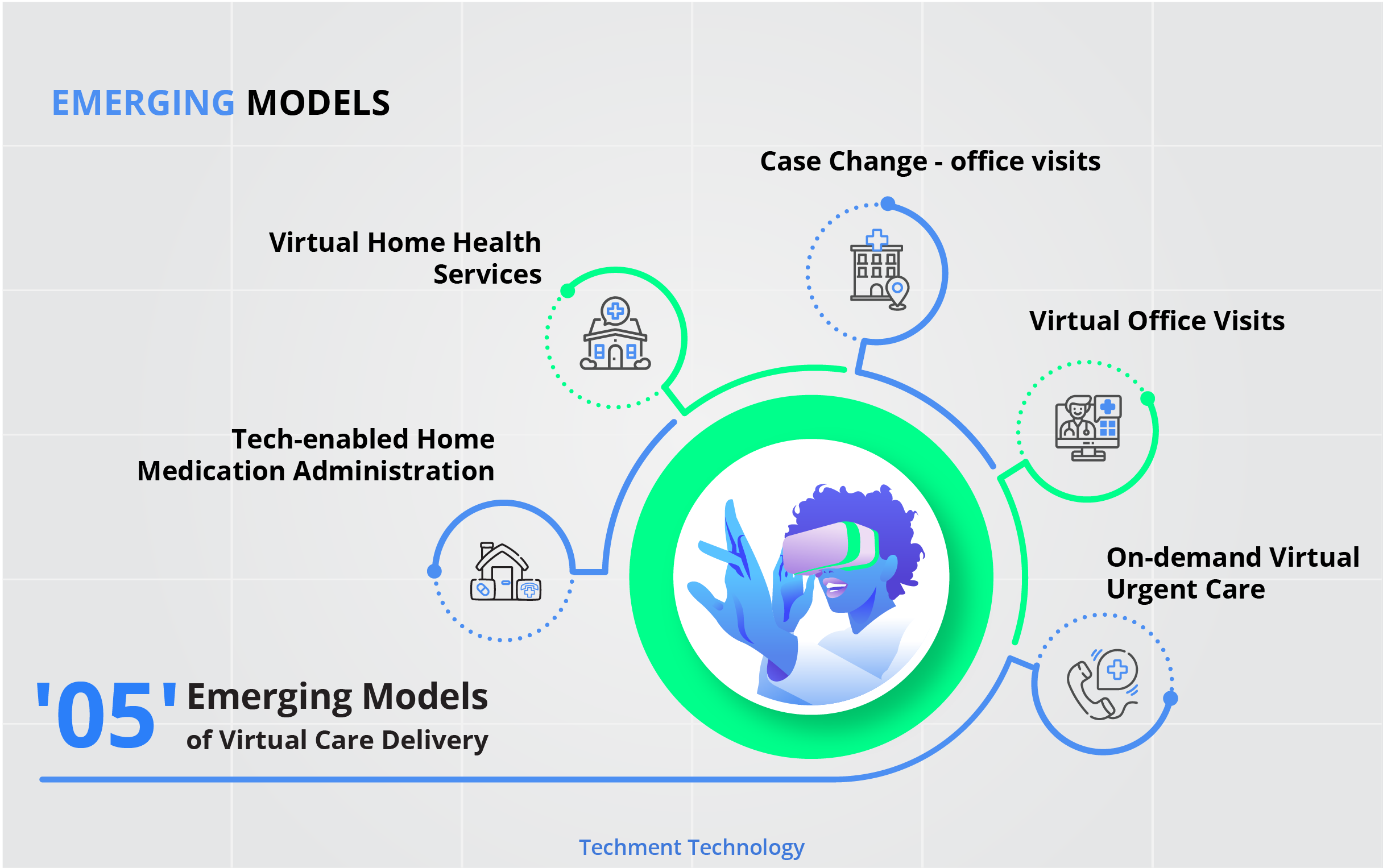
On-demand Virtual Urgent Care - These are most common telehealth use cases today and are apt alternatives to lower acuity emergency department (ED) visits, urgent care visits, and after-hours consultations.
Virtual Office Visits - Most suited Patients with chronic conditions with the support of remote patient monitoring, digital therapeutics, and digital coaching.
Near-virtual office visits - Extend the opportunity for patients to conveniently access care outside a provider’s office.
Virtual Home Health Services - Leverage digital patient engagement tools for treatments such as physical therapy, occupational therapy, and speech therapy.
Tech-enabled Home Medication Administration - Drug delivery and administration form the clinic to the home.
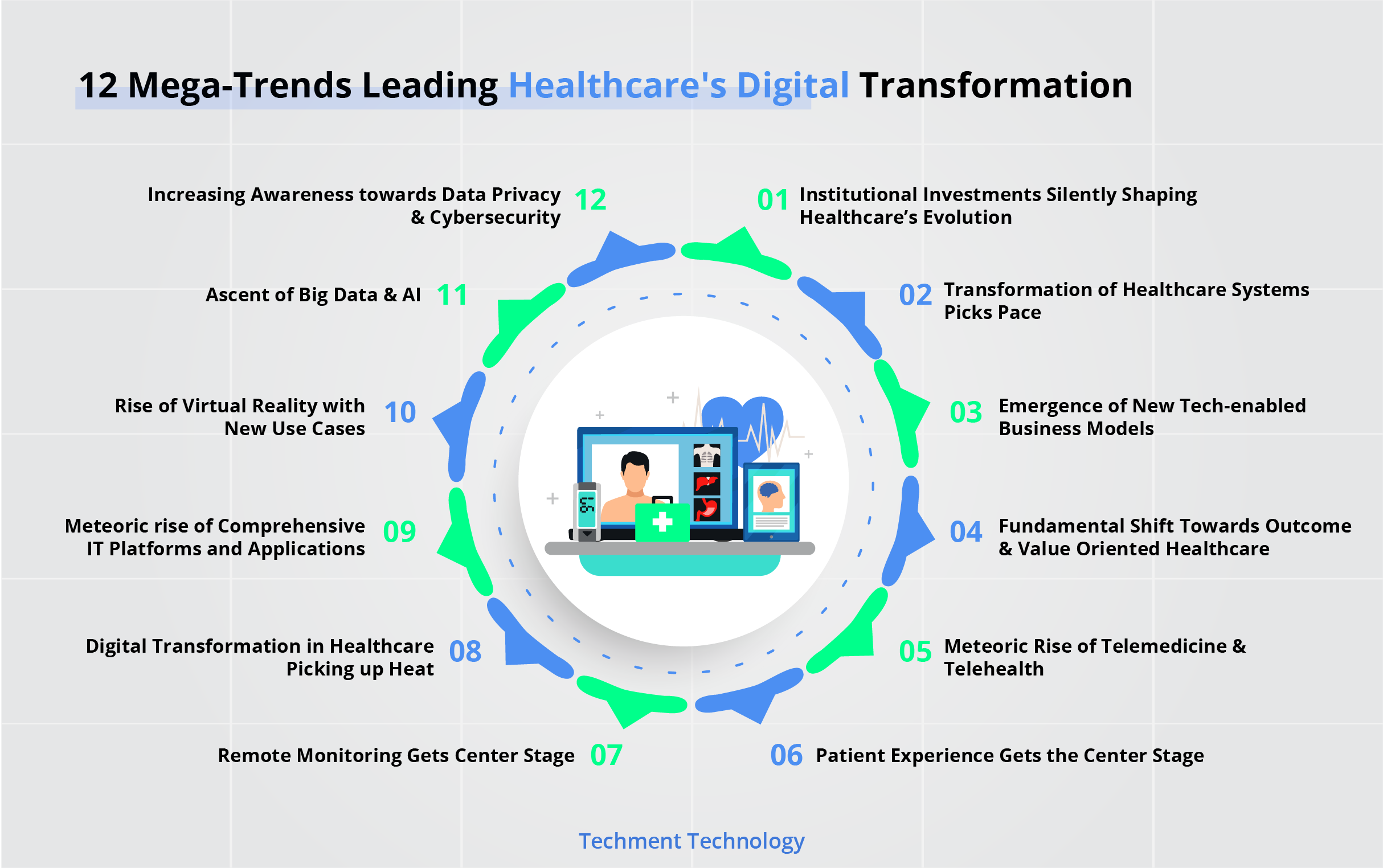
5. Healthcare Mega-Trends 2021 and Impact of COVID on Virtual Care
Increasingly, care is being shifted to non-traditional settings and to understand the changes and transformation the healthcare industry is undergoing, it is essential to look into the trends that are shaping up.
Here are the trends:
Trend 1: Emergence of New Tech-enabled Business Models
Hitherto, the innovations have focused elaborately on reducing the cost and increasing the productivity, but the results have been uninspiring vis-a-vis other industries.
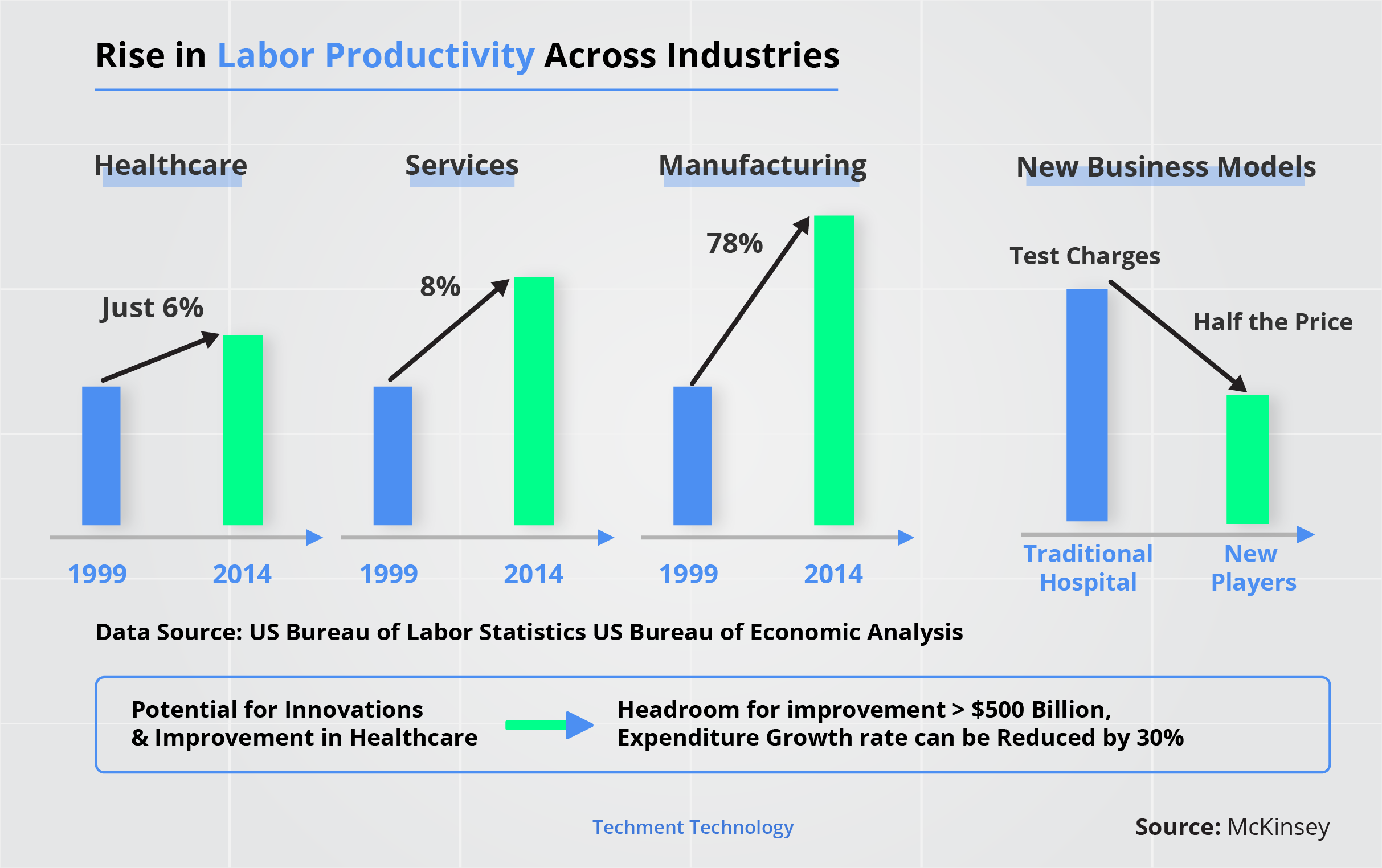
The data clearly shows that labor productivity rise has been much behind other industries.
New players such as diagnostic laboratory chains, retail health clinics, and dialysis companies have redesigned their business models to innovate and compete with hospitals.
Research estimates a possibility of improvement in healthcare that is over US$ 500 bn, and reduce the growth rate of expenditure by a massive 30%; innovations can thus benefit every party.
Some Recommended Business Model Innovations and tools:
-
Ambulatory Surgery Centers (ASCs) have ramped up productivity at lower capex and reduced costs to half.
-
Walmart Model: Providers can also indulge in innovation by leveraging technology as done by Narayana Health System, India. Its “Walmart” like approach leverages technology to boost efficiency with automated schedules and optimized operations that resulted in one-third the price of other hospitals.
-
Digitization: Payor or insurance companies can remarkably benefit from digitization that can not only save their cost of acquisition but also reduce operating cost by over 20%. But companies must be aware of the full process of Digital Transformation while they even attempt to digitize part of operations.
-
Here is our comprehensive DX framework:
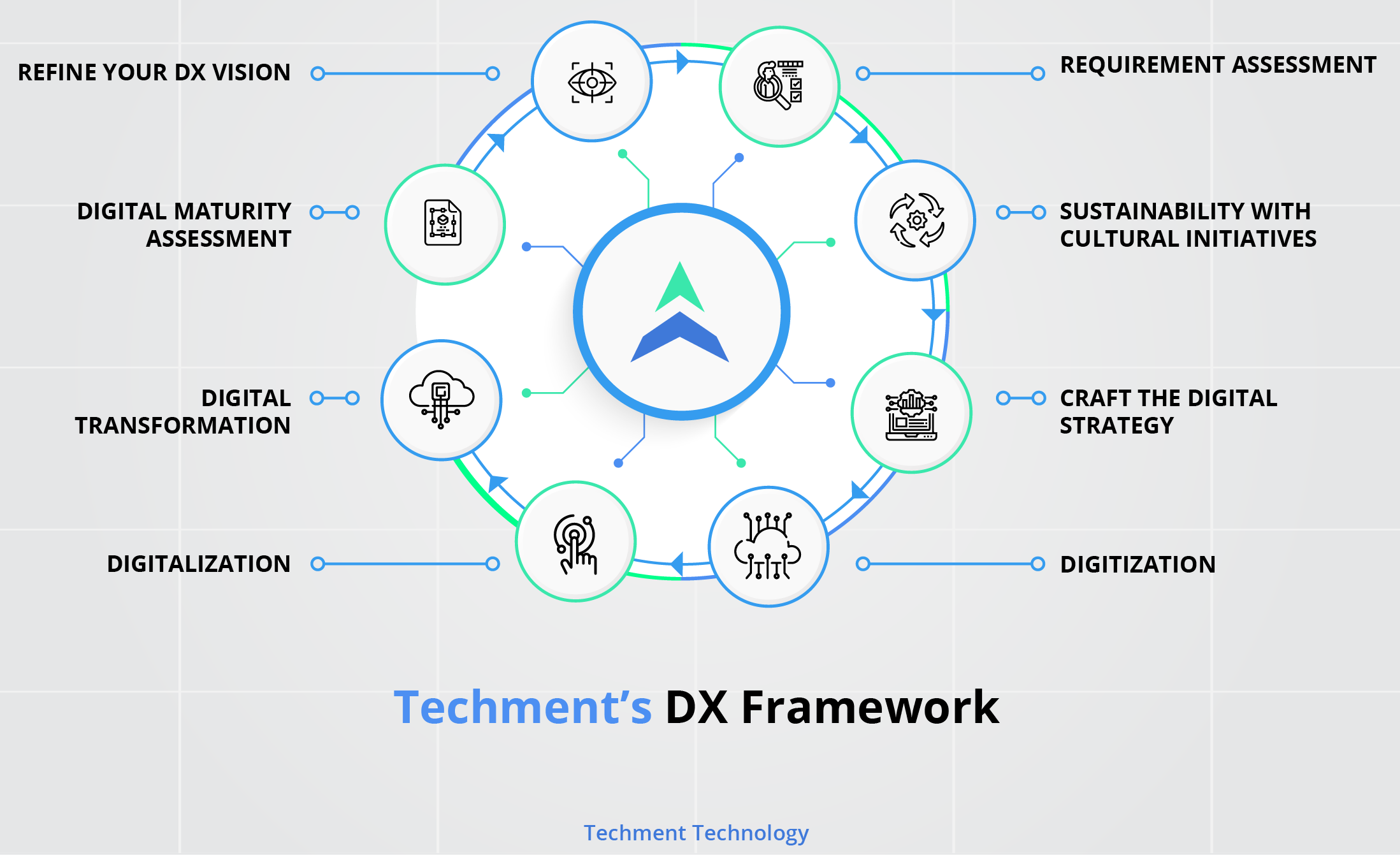
-
Hub-and-spoke Model: Restructuring the claims and payment transaction system to a “hub-and-spoke” model.
-
AI/ML: AI can improve the speed and accuracy of diagnosis, innovations and give agility
-
Remote monitoring technologies like MIoT, telemedicine reduce are more affordable as well as effetive for patients with chronic conditions.
-
Personalized medicine and treatments tailored to patients’ individual characteristics.

Are Digital Technologies going to create Innovations and New Ecosystems?

Dr Vikram Venkateshwaran:
Large-scale platforms can create new channels and markets for healthcare delivery.
Their role is even more significant as their capability to become ecosystem integrators;
bringing together different stakeholders, products and services to create and co-create value,
and allowing patients to have better access to healthcare.
- Dr Vikram Venkateshwaran
In new ecosystems the leading role has been played by Software, platforms, and technology along with Data, analytics, and information services companies. A pre-covid estimate4 pegs their growth rates at 10-12% and 16-18% respectively. In the post-covid context, the growth can be significantly higher as there are several areas where integrated platforms could add value:
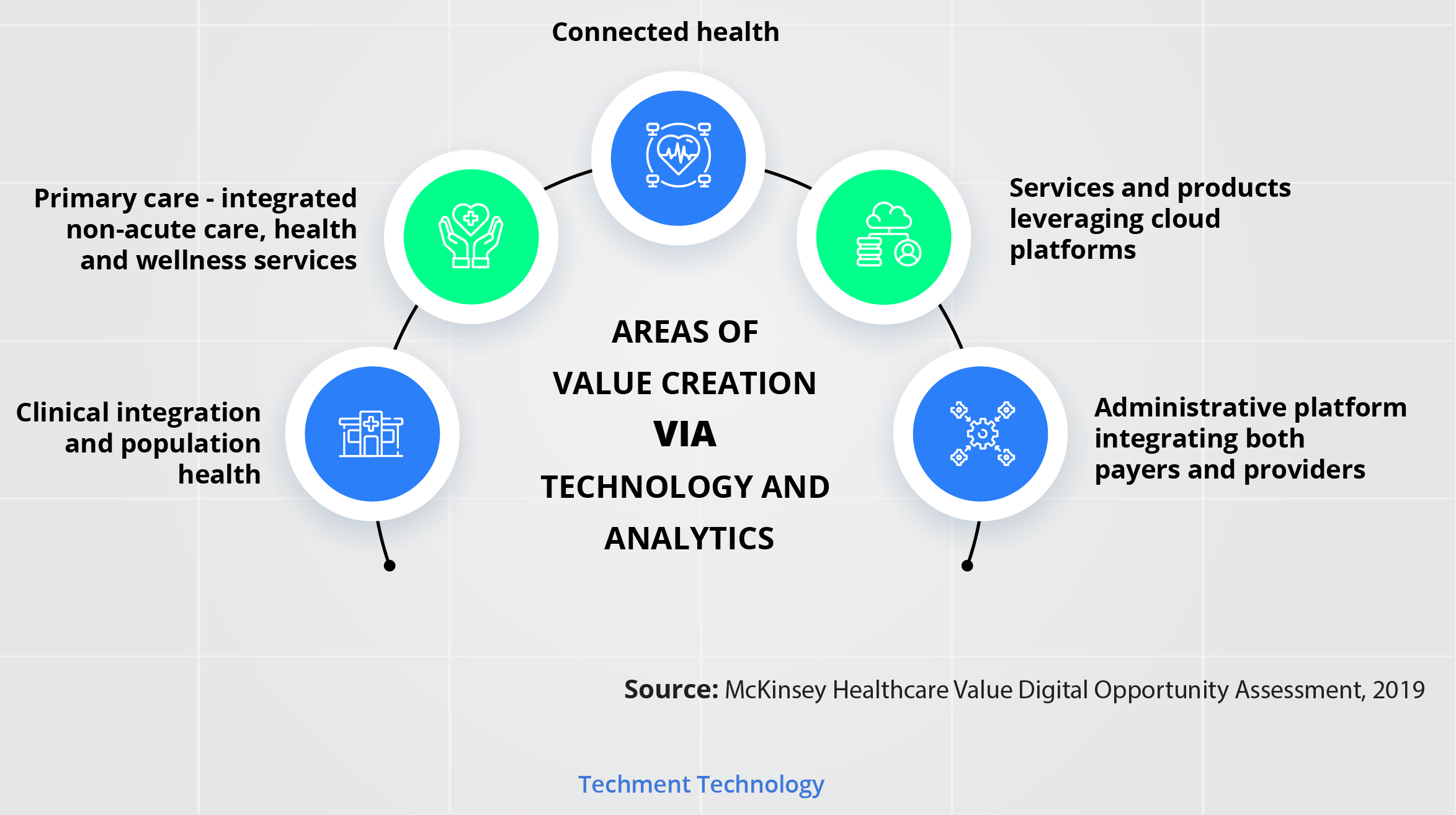

Trend 2: Transformation of Healthcare Systems Picks Pace
The techtonics of care delivery have shifted considerably, and the transformation is led by many numerous factors. We sought answers from the panel of our experts. Here is what they shared :

How do you see the recent paradigm shift and Post-Pandemic Telemedicine Momentum :

Jay H. Sanders: The paradigm shift that I have observed in 2020:
-
The Federal Government has realized that it is essential to make the system work and thus reimburse it.
-
Physicians have realised that there is no alternative to telemedicine. Most popular usages of telemedicine are - Radiology and ironically Mental Health. Psychologists who viewed telemedicine as ineffective for them now think completely differently. Seeing patients in their homes is a much better place for consultation.
-
Patients have realised that they need telemedicine as much as they need Amazon and Netflix.
-
The remote areas now have access to specialists, who can provide critical care such as heart attack, thrombotic stroke, etc. Remote care has become more relevant.

What is driving the sea of transformation in Healthcare today?

Christine K Jacob: "Data is the fuel to this transformation. Digital tools such as apps, AI, wearables MIoTs, and diagnostic devices are generating unprecedented amounts of data, by monitoring people at home, getting vital stats, and helping patients report their symptoms without coming to the clinic. Consequently, it is making possible personalized healthcare, and predictive research."
Today, patients can self-monitor, and participate in a dynamic approach to treatment as they
become part of the care. They can report, monitor, and express themselves.
Data is the backbone of the transformation that we are seeing today.
- Christine K Jacob
Companies like Apple and Google that have experience with managing data could play a critical role, but there is a need to partner with the HC companies to help with things, such as contact tracing and other diagnoses.

Trend 3 : A Fundamental Shift Towards Outcome and Value Oriented Healthcare
The Affordable Care Act (ACA) in 2010 kicked a debate on reforms on two line:
-
Expansion of insurance coverage -- Led to the discussion on Medicare for all
-
How providers should be reimbursed for their work -- Led to discussion on validity of the flawed system of fee-for-service reimbursement instead of outcome based rewards.
Ten years since ACA, only incremental progress can be seen, while concerns loom large.
Here is how our esteemed collaborators explain the shift:

Does the advent of digital puts the focus back on outcomes and outcome linked incentives?

Christine K Jacob:
As digital involves data and allows constant monitoring, it certainly puts the focus on outcomes as
it makes it easier to measure success and results with better transparency, measurement,
monitoring, and tracking. Digital is enabling the shift from patient care to health care.
- Christine K Jacob
The current focus is on curing and fixing the ailment. In very few cases do we see a holistic approach, a multidisciplinary approach, especially with people with chronic diseases or autoimmune diseases? Complexity needs monitoring and interconnectivity, else it is just separate specialists trying to fix it would not yield the best results.

With the advent of digital, will care delivery change, do you see that we are going to see winners and losers?

Dr Vikram Venkateshwaran:
The winners and losers are already there. The winners have the data and have the systems to harness it, analyze it, and use it to deliver better outcome oriented care. Many non-traditional healthcare organizations that are generating and using data will take giant leaps forward.
The loser will be those that can not either harness data or do not even have data. The Biggest losers may be the hospitals that do not change and are very rigid right now.

Trend 4: Meteoric Rise of Telemedicine and Telehealth - Is the Trend Here to Stay?
A study5 of 16.7 million medical visits in 2020 revealed an astonishing 2,000% increase in telemedicine visits. Much of the dynamics is likely to sustain for at least the coming year and consumers’ preferences for care access will continue to evolve, and virtual health could become more deeply embedded into the care delivery system.
The technology holds immense future potential as more progressvie regulations are expected in the post-pandemic scenario.
Unravelling the Future of Telemedicine
Telehealth has incredible potential in areas such as behavioral health, improving the patient experience, and bettering health outcomes. Incorporation of virtual and near-virtual health solutions takes healthcare to homes, enabling patients to access timely care. He spoke on the paradigm shifts, technology, regulations, medical errors and more. To listen to the entire interview click here.
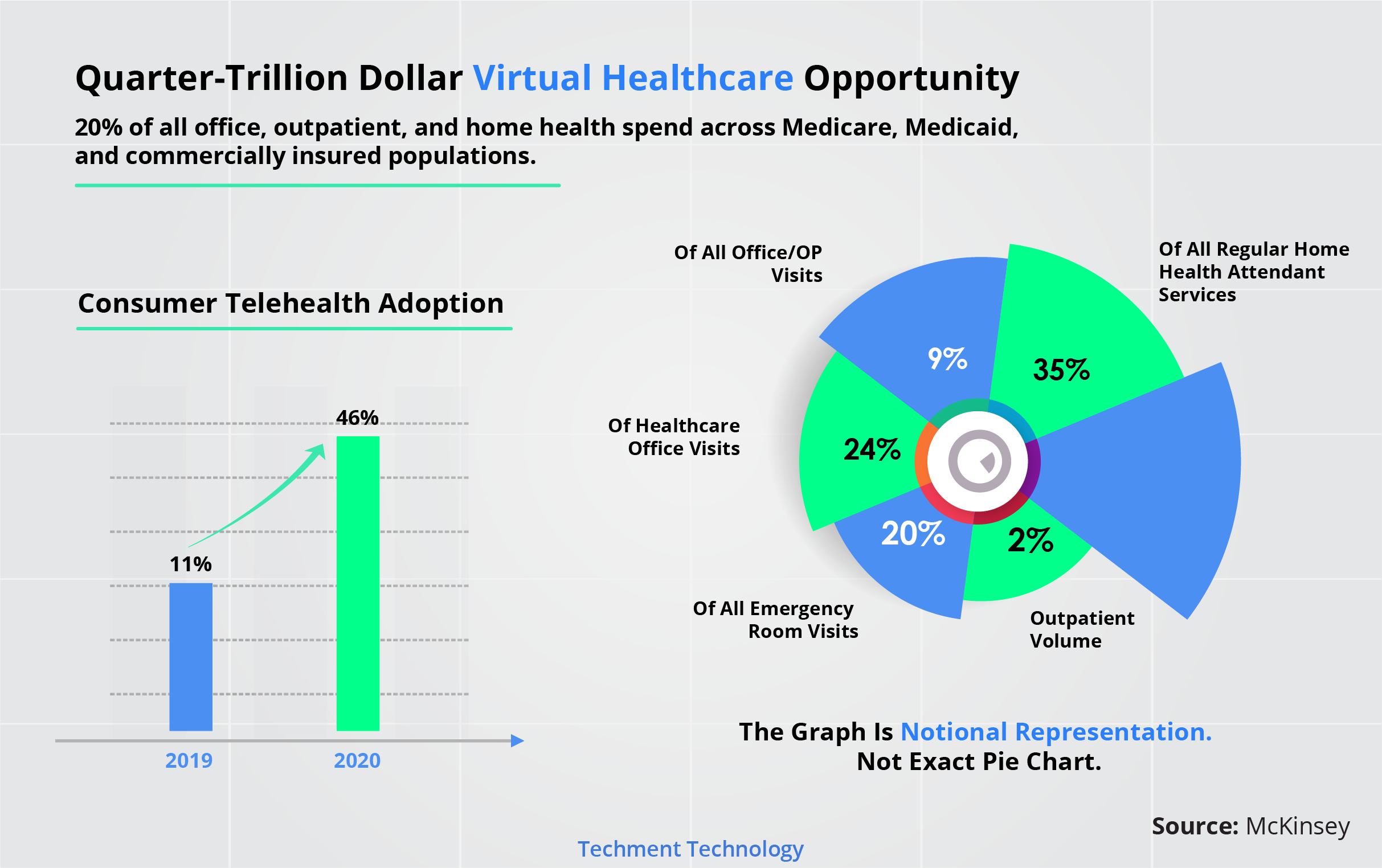
Excerpts from the Interview :

What is unique about the telemedicine adoption and will the telemedicine momentum sustain?

Jay H. Sanders: “I have been dealing with Telemedicine for 52 years, and fundamentally, the things which have prevented its mass adoption are Regulations and Insurance companies not reimbursing for it.
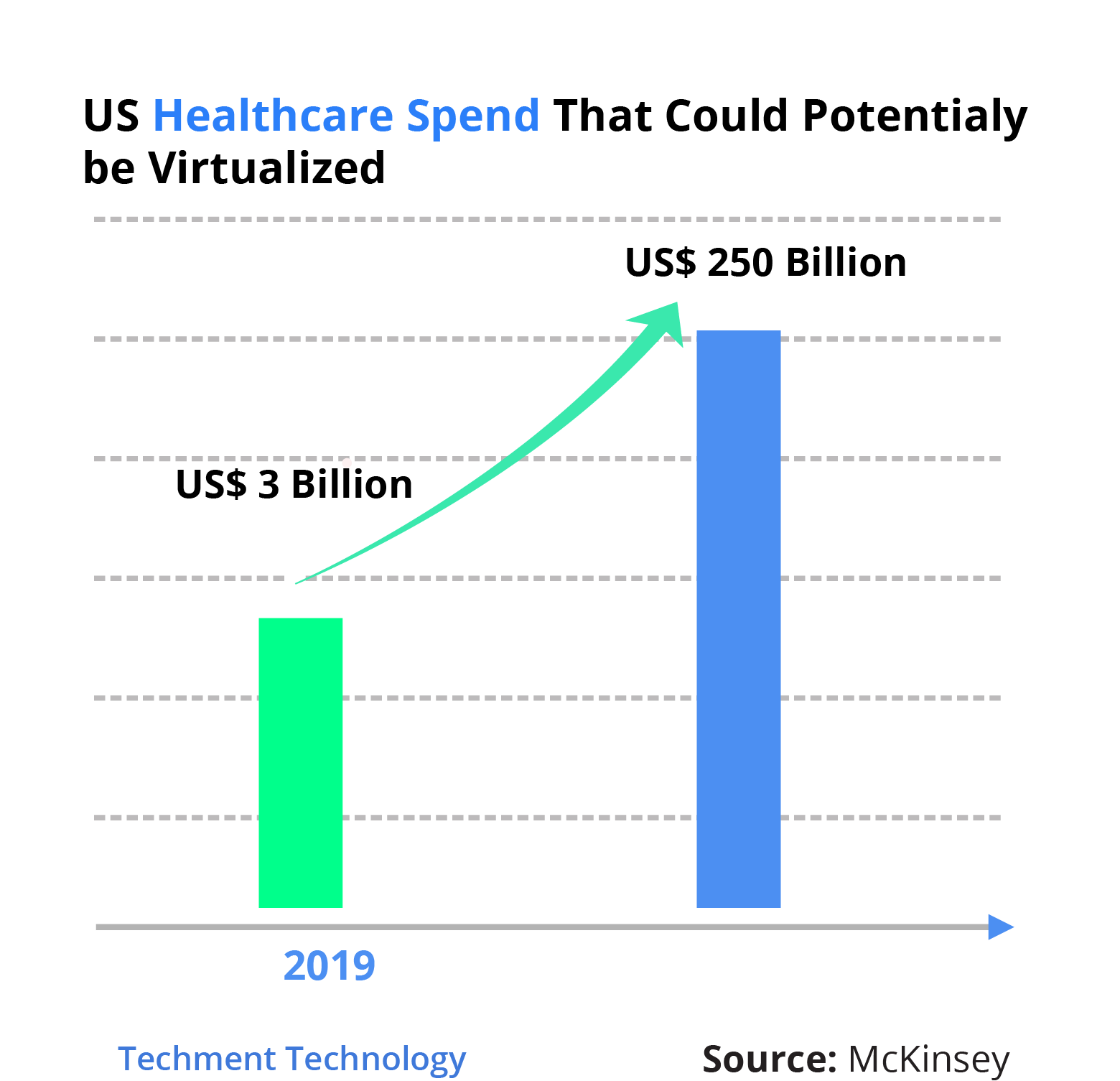
The case of Telemedicine is similar to that of companies like Amazon, Netflix, and online banking ones that gave customers an alternative to shop and bank. It did not shut the malls or the banks, it added additional value.
- Jay H. Sanders

Moving forward, do you see Regulations impeding tech innovation ?

Jay H. Sanders : Finally everyone has seen the light wrt. to the capabilities of Telemedicine. More than 30 states have legislated parity reimbursements, i.e pay at par with regular hospital visits, such legislations are good examples of progressive adoption.

Would Reimbursing Telemedicine visits Benefit Insurance Companies?

Jay H. Sanders : Even if insurance companies decide to pay at par, they will still be able to make money because many people consider the emergency wing as their regular physician. They go there when they do not actually have an emergency, and then the insurance company has to pay many times more than a regular visit.
Nearly 30-40% of patients who come to the emergency department never need emergency care, so telemedicine can save a lot of money for insurance companies by addressing emergency care.
- Jay H. Sanders

Would Technology contribute significantly to reducing medical errors, thus saving lives, costing billion of dollars?

Jay H. Sanders:"We lose more numbers of people each year due to misdiagnosis and error than we have lost to COVID. Technology can help change that!" Jay H. Sanders
There is enormous pressure on institutions, doctors, workers, patients and communities and it is impossible to keep up with the latest advancements and research. Here is the urgent need for AI to assist them with the latest information, and provide an alternative diagnosis.
We need technology and automation to replace the single physician at bedside with collective expertise through telemedicine and AI.
Also, Sensor technology should tell us what’s wrong with a person, as each has a different normal and only the sensor can tell us anomaly for each person.
Future Tech : 3 Most Important Technology that Will Change Healthcare : Telemedicine enabled with AI and sensor Technology.


How do you see the darker side of Telemedicine - The Risk of Misdiagnosis?

Jay H. Sanders : There are many cheap MIoTs (Medical Internet of Things) and diagnostic devices available which can aid the consultation and reduce the chances of error. Thus physicians today can leverage diverse devices to eliminate the risk of error of judgement.

How does the overall future of telemedicine look?

Jay H. Sanders : We may expect a little positivity and change on the regulatory front, as it holds the key. But we are still far from its true potential, and only with incorporation of AI, VR/AR and automation shall we see it changing healthcare radically.
Trend 5: Patient Experience Gets the Center Stage
The ability to connect with a doctor at any part of the world, suddenly takes the competition to another level. With presence of MIoTs, diagnostic instruments, and high connectivity networks, it is possible for doctors to diagnose with high accuracy.
We spoke with our panel of experts about what they think about patient experience as the center of a new care delivery model.

Apart from the use of data and analytics, do you see the paradigm of seeing patients as customers and focusing on patient experience as a factor that becomes the core differentiator between healthcare providers?

Dr Vikram Venkateshwaran:
Yes! The whole paradigm is changing, from an intervention based medicine to preventive medicine. So the need for a massive intervention is spread across time in the form of smaller interventions and checks. Hospitals will change their function by moving from one stop intervention provider to an organization that partners throughout. -Dr Vikram Venkateshwaran
Healthcare is coming to the patient via mobile, connected devices, and more. The patient experience will thus be the prime focus.

Does 2021 mark the rise of patient experience in the same way as customer experience in other industries?

Helen Yu : The rise of patient experience will catch up with the hype of customer experience in 2021. Institutions will pay more attention to patient experience in 2021 due to the pandemic. People will have more empathy for patients, especially those who had suboptimal experience.

Moving forward, do you think patient experience would become as important as customer experience in other industries?

Christine K Jacob : The constraint of insurance companies who do not allow to switch between providers would hold the exigency of the focus on patient experience. But for those who can switch, yes, it would be significant. In countries like Germany and Switzerland, where you can pay additional for extra options to choose from, patient experience is vital.
But without choice, it would take time, and we need a mindset change to allow the competition on grounds of personalization, options, telemonitoring, telehealth, and enabling consults from home. But when incentives such as reimbursement are not available, we would face a barrier to adoption. In such a case, the willingness of patients alone is not enough; even when they are ready.
Trend 6: Digital Transformation in Healthcare Picking up Heat
The digital platforms enable organizations to break the old shackles of creating value within the boundaries of their firm and supply chain by orchestrating a new ecosystem in which a much wider array of stakeholders create value together. In contrast to other industries which have leveraged digital platforms, the healthcare industry has lagged behind in creating this interorganizational perspective.
The sheer complexity and regulation of healthcare industry has resulted in information silos and lack of interoperability of health IT among key stakeholders which thwarts efficiency, impedes coordination of care, and ramps up the costs (Gupta and Sharda 2013; Hansen and Baroody 2020; Kellermann and Jones 2013).
Digital Transformation Trends in Healthcare
The revenue fall7 also pushes health systems towards value based care, this also motivates a shift from volatility of volume-based reimbursement towards capitation reimbursement models that enable more predictable income.
Digital transformation in healthcare will create inter-organizational partnerships in ecosystems as value is co-created among diverse and new stakeholders (Jacobides et al. 2018). Additionally, technological advancements have made services and technology companies the fastest-growing profit pool in the healthcare industry.
Latest research8 that studied the digital transformation of 1830 healthcare organizations identified 8 new roles within healthcare:
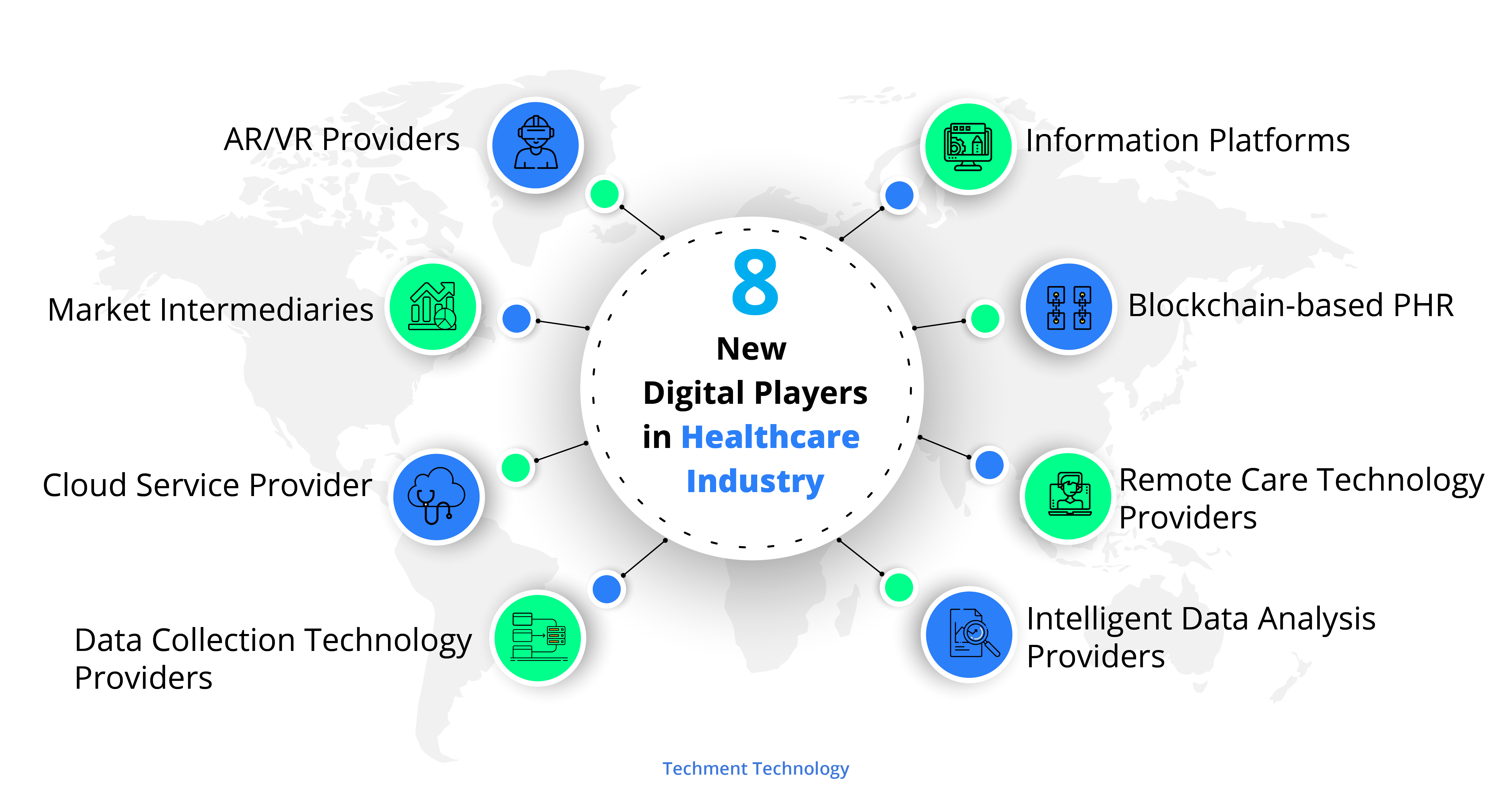
The new dynamics is interesting, the competition between new entrants and incumbents, will create innovations and contribute to the changing role of patients, transform value proposition and delivery. The areas in which there is a need for digital transformation:
-
Payment Gateways and Options : Most have or are in process of having digital payment options to boost their satisfaction and lower the costs. An earlier survey9 reveals that only 20% were ready for digital payments.
-
Collections and Back-office Processing :
Administrative costs in the U.S. are massive 8%10 of total healthcare spending vis-a-vis a global average of 3%. Electronic solutions can negate the time-intensive, error-prone back-end and collection processes by automating them, offering tremendous opportunities to increase efficiency and lower costs for industry stakeholders.

How would be the digital transformation and tech incorporation in healthcare be different from other industries ?

Helen Yu:
-
In a recent survey done by digital authority partners, only seven percent of healthcare and pharmaceutical companies said they had gone digital, compared to 15 percent of companies in other industries. Healthcare moves slower when it comes to adapting to digital.
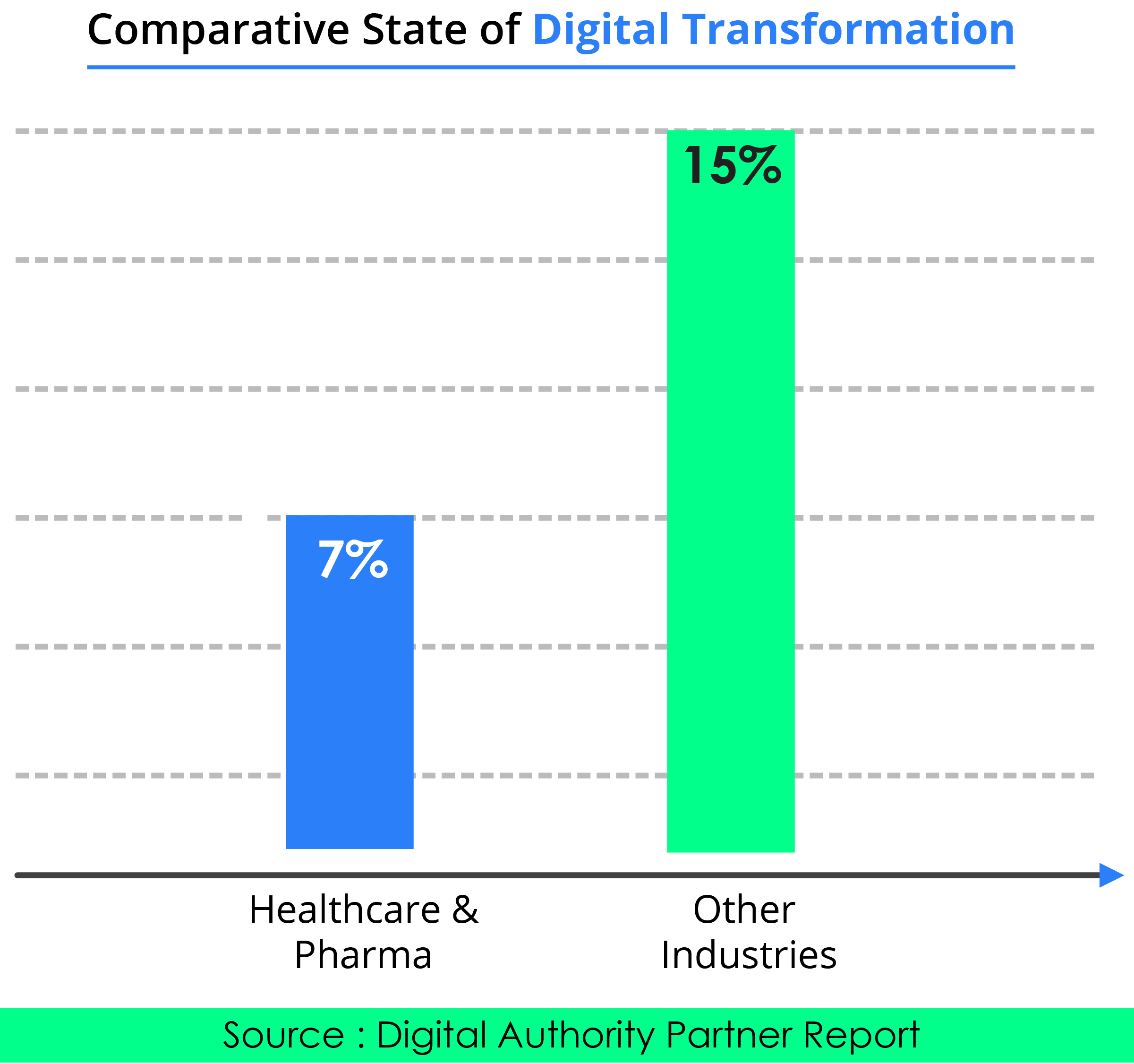
-
Healthcare is more complex and highly regulated than most other industries because of the sheer diversity of players involved from physicians to care facilities that are governed by state agencies, policymakers and credentialing entities involved.
-
Keeping up with digital transformation in healthcare can be overwhelming, because many aspects could be out of your control. To digitize any process, you have to understand the current processes, the downstream and upstream impact of those changes. And if the digitized process is in compliance with regulations.
-
Privacy concerns. A 2019 Gartner survey found that 40% of healthcare CIOs plan to spend new or additional funds on cybersecurity tools in 2020. According to Palo Alto Network, due to the long life cycles of medical devices, medical IoT devices are among the worst offenders of running outdated and, in many cases, end-of-life operating systems. These devices are neither maintained by IT nor supported by the operating system vendors.

We are seeing a radical and fundamental shift in Healthcare systems. What according to you has changed quintessentially ?

Dr Vikram Venkateshwaran :Four factors are driving the digital transformation:
-
The expectation of the patients has changed and is the biggest driver for digital transformation.
-
The pandemic proved a great catalyst!
-
People are now holistically seeing health and taking responsibility for their health. This makes everyone a consumer of healthcare services because now the objective is not to fall ill.
-
Today the care delivery model has changed; a patient does not need to wait for his doctor as he can seek an appointment online and get diagnosed from his office. Innovations in the care delivery model are happening. Patients can now consult a doctor overseas and his care would be delivered by a local hospital. AI is also driving much change by helping in diagnosis.
Organizations are transforming to serve the larger market.

What unique challenges do you foresee when healthcare institutions such as clinics, labs, hospitals begin their journey of digital transformation? (Especially SMEs.)

Helen Yu:
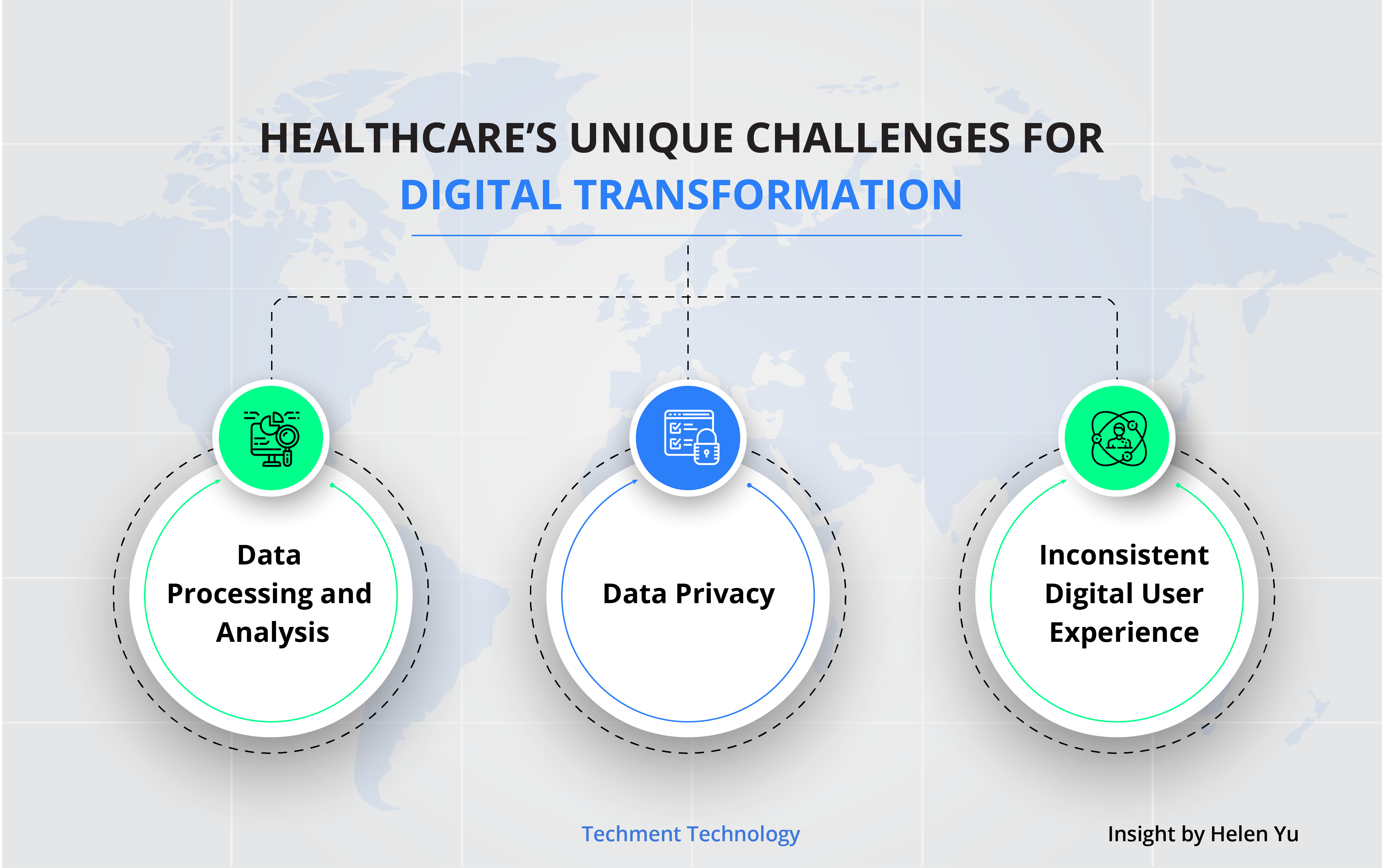
-
Data processing and analysis is challenging due to the sheer amount and complexity of data collected. AI can be leveraged to analyze data in order to deliver better and more personalized care to patients.
-
Data Privacy - a study by IBM revealed that healthcare organizations had the highest costs associated with data breaches, which were three times higher than in other industries. This means healthcare must invest in cybersecurity and ensure QA process before the launch or update of products and systems.
-
Digital user experience is inconsistent due to lack of standards in the healthcare ecosystem of connected devices.

How much time do you think the hospitals have to go digital?

Dr Vikram Venkateshwaran:
-
It will take 5-10 years. Data storage poses a formidable challenge as it is highly expensive. Hospitals compress data to save costs resulting in errors when data is used for analysis and when AI is deployed.
-
The biggest challenge is the interoperability of the systems; they do not speak with each other and hence, can not share the information and fail to leverage the data available.
-
Another challenge is the lack of standardization of SoPs that today are experience-driven.
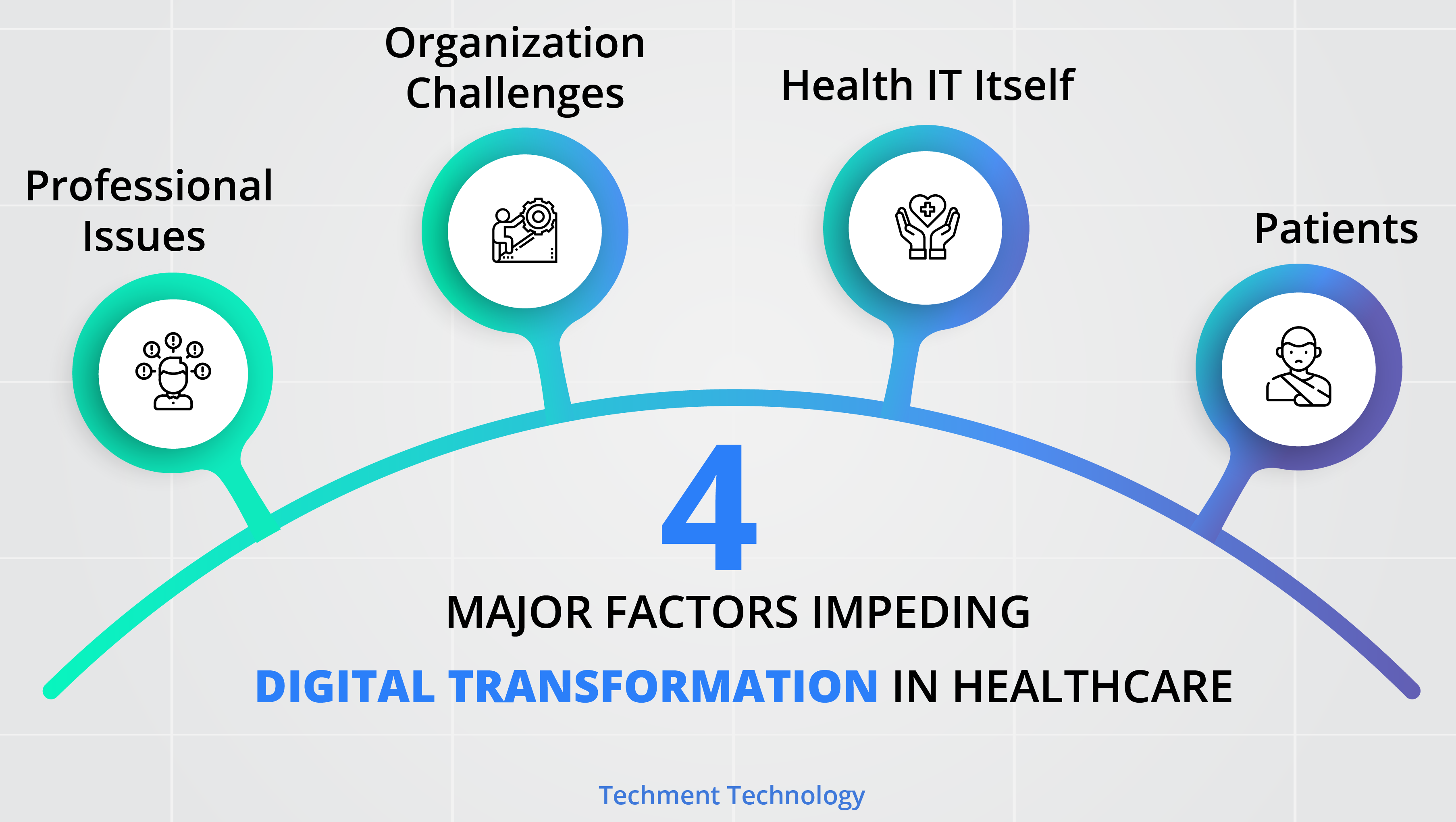
a. Professional Issues
-
Professional Perspective - Doctors focus only on patient treatment, and consider rest as administrative nuisances
-
Negative Influence - Many tech-averse physicians discourage others
-
Privacy Concerns
-
Application’s Opaque Privacy Policy
b. Organization Challenges
-
Absence of incentives to implement health IT systems
-
Initial and ongoing costs
-
Technological support and Apprehensions
-
Fear of Technological Obsolescence
-
Poor Adoption upon implementation
c. Health IT Itself
-
Only few build easy to use products
-
Many require data entry and disrupt workflow
-
Validity of diagnostic devices, sensors is a concern
-
Opaque privacy policies
d. Patients
-
Lack of trust in sharing personal medical information
-
Not all are tech-savvy
IT Advancements are Addressing Above Challenges
Significant advances in IT have been made in terms of collection, storage, processing, analysis, and distribution of data enabling new forms of healthcare.
-
Better data collection with wearables
-
Advances in health platforms solving interoperability with data sharing ex. Apple Healthkit and Google Fit
-
Cloud Computing is solving storage, processing, and capex challenges. Amazon Web Services is one such platform
-
Advances in AI/ML, NLP help in better analysis and discovery
-
Telemedicine and remote care platforms have become highly effective
-
Also, progresssive policy stance is creating a favorable ground
-
Lately, Venture capital and institutional investments are focusing on DX aggressively
Trend 7: Meteoric rise of Comprehensive IT Platforms and Applications
Countless companies have announced their foray into healthcare because now it is centered around the patient. Like in other industries, “Single Pane” view of the entire patient journey has become paramount with the rise in the number of touchpoints and data inputs.
To ensure patient experience, various health systems have begun seeking out solutions similar to SRMs to address workflows and other unique challenges of patient engagement with better overall control.
New platforms enable patients to interact, share data, get notifications while giving organizations the ability to see their entire journey– medical history, insurance, scheduled appointments, preferences – all in one place.
But all is not so rosy, many of these applications fail miserably and create more pain that value
Designing Perfect mHealth Applications
The complexity of healthcare technologies is
more profound than the apps or tools that address a
single user need because they involve patients with
comorbidities that can be treated only with
multidisciplinary teams working across organizations. EHR is an example of ill-considered technology incorporation that, instead of adding value, caused harm to the entire system.
A mHealth application may be very crafty, but can still fail miserably because of lack of adoption by clinicians/patients and thus every healthcare institution
as well as other players planning to develop/adopt an application, must be closely aware of the factors that influence technological adoption.
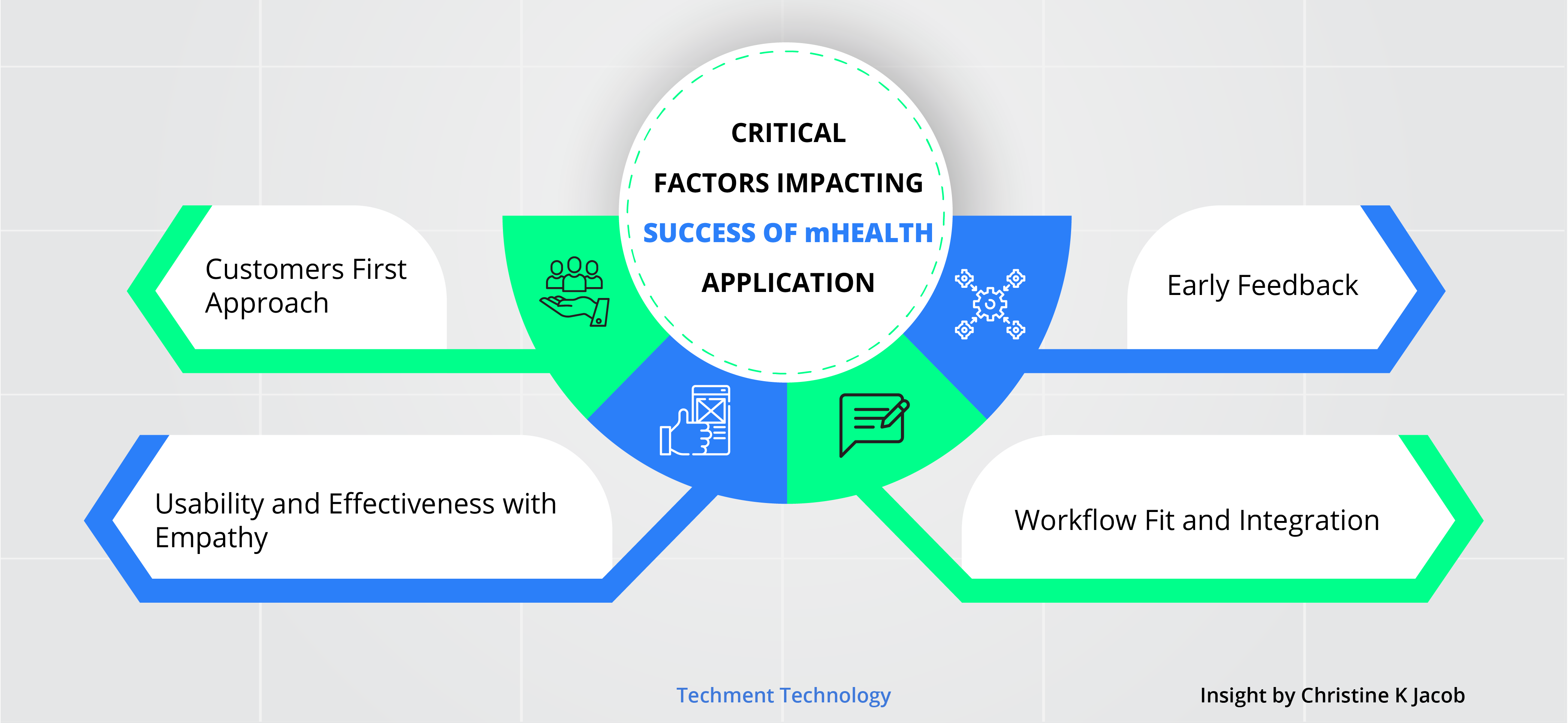
In Conversation with Christine K Jacob, the founder and Managing Director of Digi-Bridges, who is an expert in User Adoption Research and User Engagement Strategies. Her research11 disambiguates the factors that influence technological adoption in healthcare, as illustrated in the graph below.
Factors impacting the successful adoption of mHealth tools
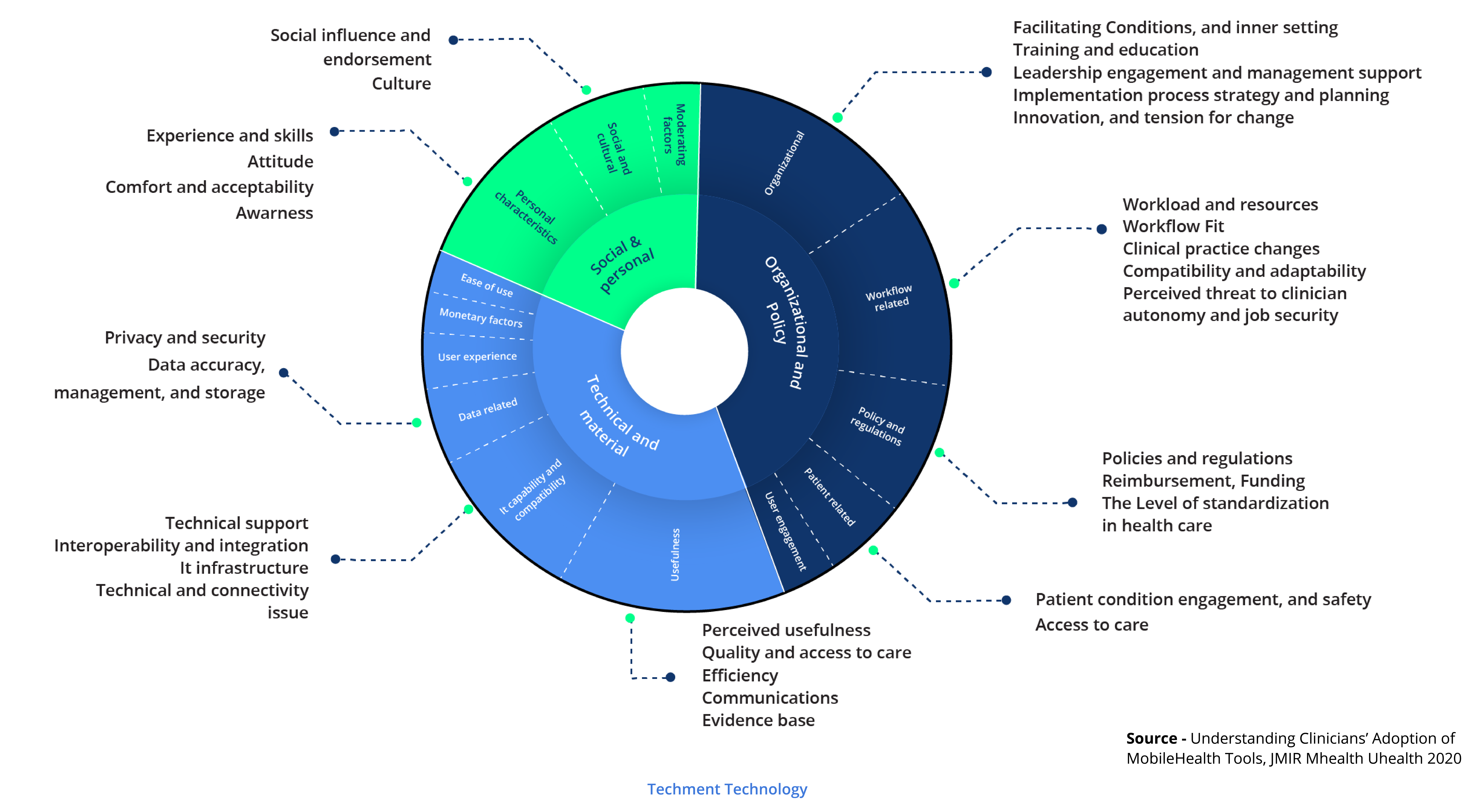
Excerpts from the Interview:
What are the factors that ensure an application’s success and what startups and other companies should keep in mind while developing the application ?
Christine K Jacob:
Companies must be mindful of these critical factors while designing their tools or applications:
-
Customers First : They should first speak to their customers. Various startups I have worked with have great technology but they have not spoken to the patients, and that poses a great risk.
-
Usability and Effectiveness with Empathy : Understanding the user’s needs is critical in making the application easy to use and effective. An empathetic approach is needed, for instance, for cancer and chronic illness patients their condition may not allow them to use the app. You have to fit into the lives of the patients and cater to their very specific needs and keep that in mind while designing the application
-
Feedback : Companies need to talk to the users at an early stage to know what they want, to develop the right product. User feedback will help to identify the problem; sometimes, it is just the design which confuses them, and they drop out.
-
Workflow Fit and Integration : When making a tool for clinicians, one must be careful to ensure that it fits into their workflow and is not an additional task; they would not use something that adds to their effort. Also, look into infrastructure; the systems need to speak with each other.
Embed the user at the heart of the development process, and make sure that every part is working together and that you are offering them enough training to be able to use your tool. Also, for clinicians and physicians, not only how to use the tool, but also seeing how it fits into the overall picture, integrating it into their workflow will go a long way in augmenting the efficacy of the application.
- Christine Jacob

Do you see the need for the role of IT platforms change to deliver better care?

Helen Yu :"The current IT platforms simply automate old and inefficient processes. The patient centric new healthcare system needs the IT platforms that cater to patient outcomes and reimbursement for creating value." - Helen Yu

Do you think that digital is also enabling personalization of Healthcare?

In many cases, outcomes can be radically improved with personalization, and digital has the capabilities to deliver it. It need not be advanced technology, but simple ideas with digital tools can go a long way in improving Healthcare delivery. For instance - Cancer drugs dosage need to be adjusted to the changes patients are facing - such as weight gain or loss; a dosage calculator at point of care can tremendously help clinicians to adjust the doses according to the patient at hand with minimal time and effort.
Another example, a doctor in France who created a tool that helps him monitor lung cancer patients with smart algorithms that enable him to identify any irregular symptoms that may arise in between clinic visits and bring-in such patients for earlier examination to deal with their irregular symptoms, and as published in several of his studies this mechanism enabled him to prolong overall survival by about seven to eight months, great results with a seemingly simple idea.

Trend 8: Remote Monitoring and Patient Engagement Become Integral
Prior to COVID-196, virtual health adoption was highly concentrated in synchronous telemedicine, not leveraging the full range of virtual health technologies. Leaders cited remote monitoring as a key area for future investment; also patient engagement was an emerging priority, now it would be even more exigent.
The pandemic has underscored the focus on the other and equally vital part of virtual healthcare.

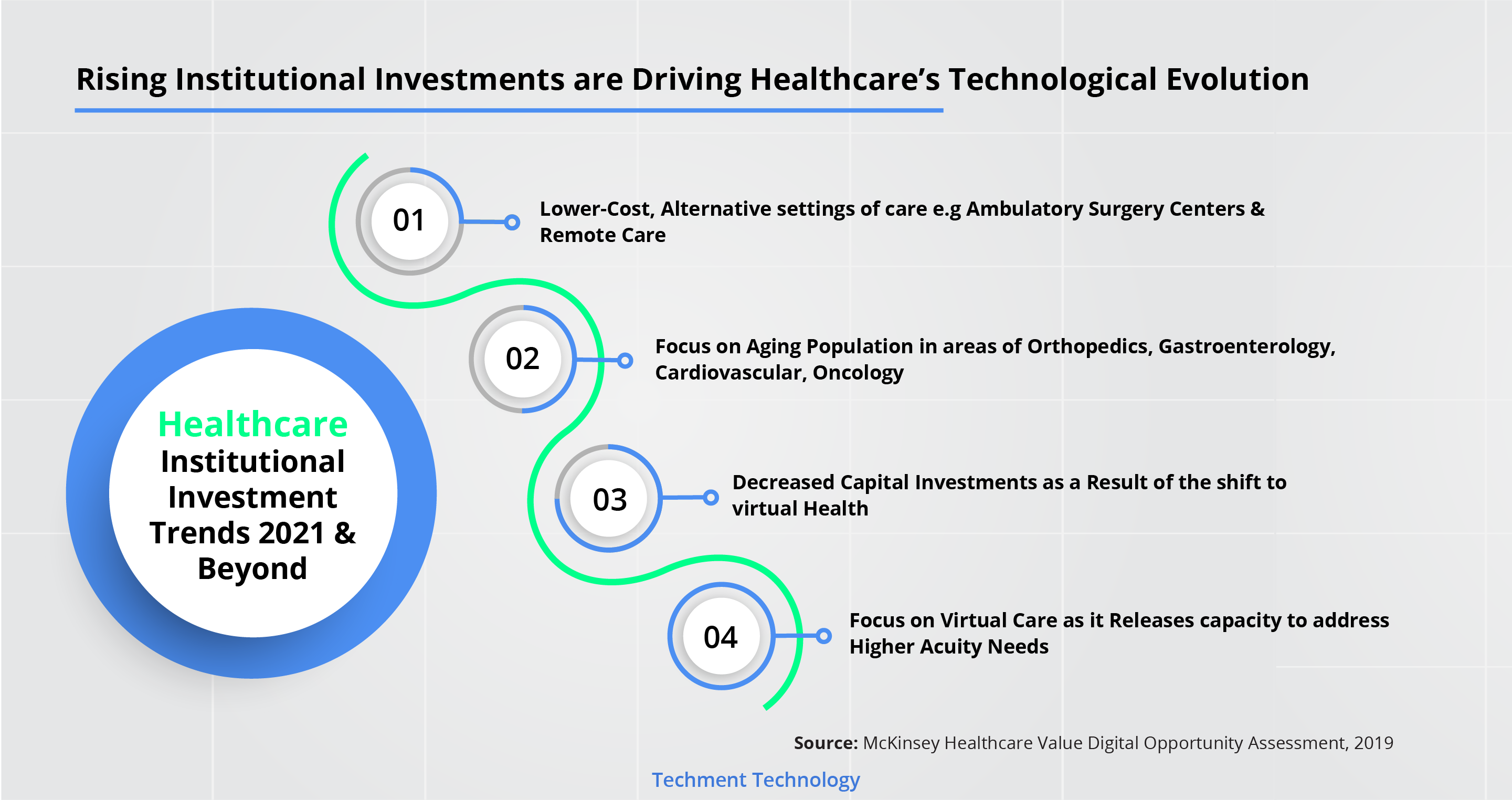
Trend 9: Institutional Investments Silently Shaping Healthcare’s Evolution
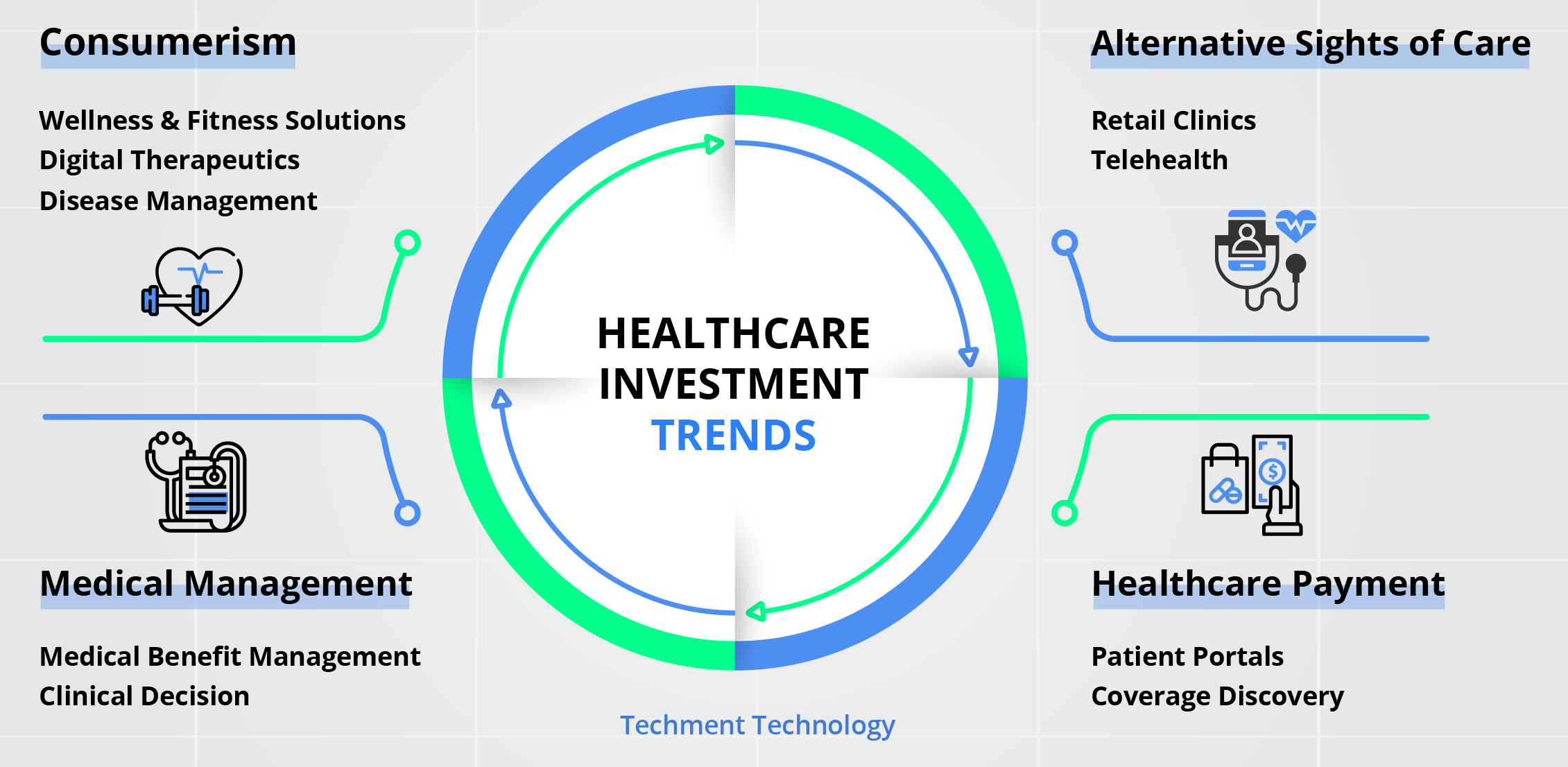
Research reveals that the nascent trends of institutional investments in lower-cost, alternative settings of care for example, ambulatory surgery centers and remote care is expected to gather unprecedented momentum.
PE, VC have grown at 16 & 19% between 2012-17. Healthcare EBITDA (2012 - 2016) grew faster vis-a-vis the combined EBITDA of the top 1,000 US companies, this explains the investment surge.
These new investments have the potential to drive structural shifts in direct ways.
Trend 10: Rise of VR with New Use Cases
Taking pain management for instance, 50 million12 U.S. adults had chronic pain in 2016. VR is a safer and better alternative to drugs for pain management; it is helping people suffering from a range of ailments, from anxiety to post-traumatic stress disorder, and stroke. VR also trains doctors for complicated surgeries, helps autistic children learn to navigate the world, in treating Bipolar Disorder and more.
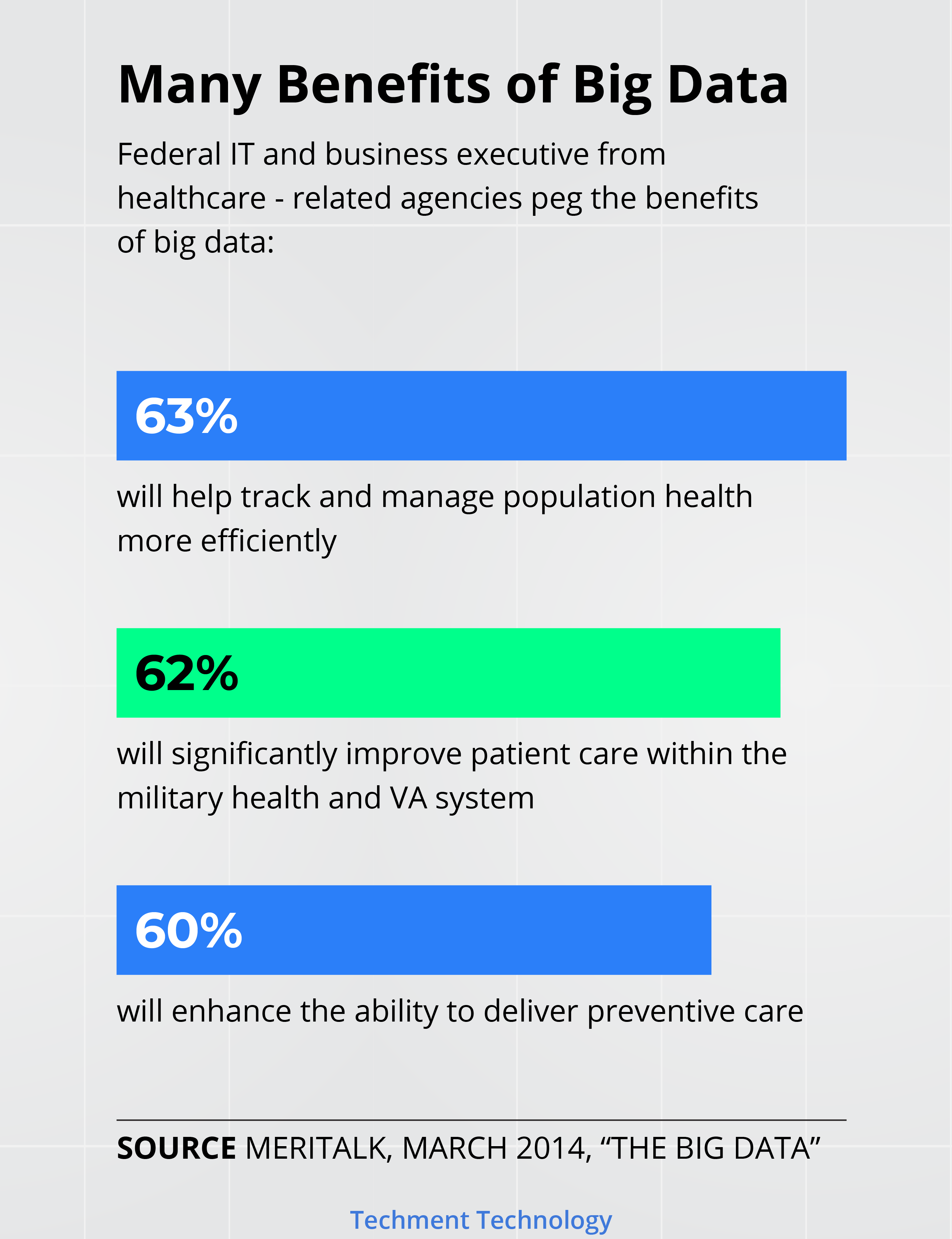
Trend 11: Ascent of Big Data and AI
Benefits of Big Data are no mystery, in healthcare it can help in following ways:
-
Lowering Rate of Medication Errors
-
Facilitating Preventive Care
-
More Accurate Staffing
-
Predictive Analysis
-
Improved Personalized Treatment
One main reason that big data has not picked up is the lack of standardization of data that has been a long-term challenge for healthcare providers, working with the most complex and disconnected data sets.
AI is helping in many ways, from diagnostics to chatbots to drug discovery. Its aggressive use will definitely keep adding value, though ethical concerns must be addressed collectively.
Trend 12: Increasing Awareness towards Data Privacy and Cybersecurity
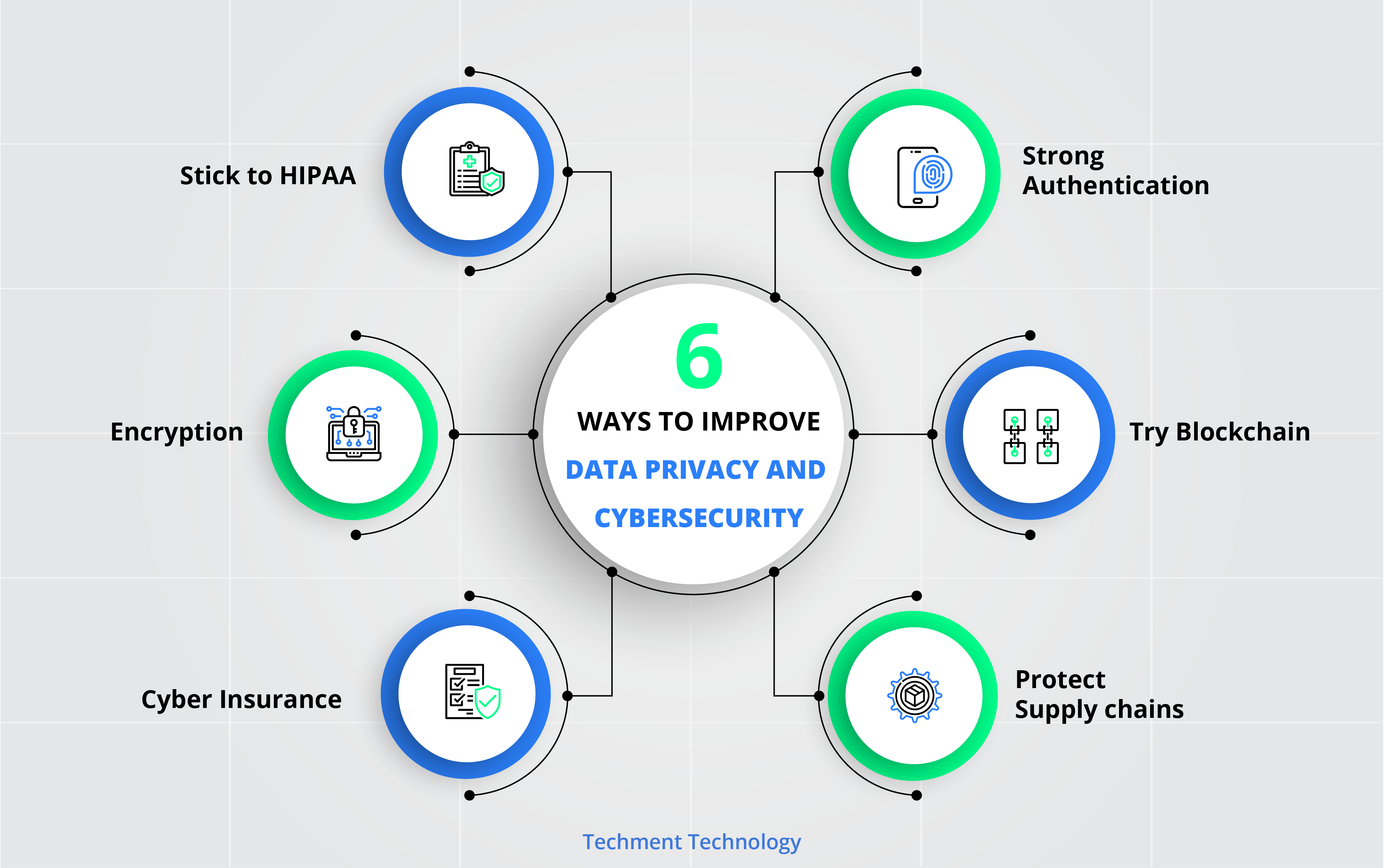
With other industries changing and upgrading to prevent cyberattacks, healthcare becomes a relatively easy target for data theft. It is understandable to share the skepticism, but care professionals need to embrace digital along with how to be safe and secure. Typically, healthcare organizations have smaller security budgets and teams which makes them prone to sophisticated attacks. Here is what they can do to protect themselves :
-
Stick to HIPAA. The HIPAA Security Rule and Privacy Rule robust frameworks to follow.
-
Encryption. Care providers should install strong encryption to all patient data and give very limited access medical charts.
-
Cyber Insurance. It is an evolving, but useful thing to consider.
-
IT Training. To prevent phishing attacks care workers must be aware of information security best practices.
-
Strong authentication. A multifactor authentication like in financial services
-
Try blockchain. Efficient, verifiable and permanent record keeping
-
Protect supply chains. They are tempting ways for criminals to gain access
The Way Forward
For a long time, we wanted to shift from acurative to a preventive and holistic medical care system. It took a pandemic for us to come close to achieving that dream through technology. Digital therapeutics, wearables are helping people prevent chronic conditions by monitoring their conditions, and through predictive analysis. We spend 10% of our GDP on healthcare, with developed nations spending as much as 70 times those of poor-nations. Digital technology will go a long way to establish a little equitability and solve the Iron Triangle by making care effective, affordable, and accessible.
The aging population, mental health, and other areas have a lot to gain from remote care, as it not only provides them better, affordable, and more accessible care, no alternative gives them so much power and control over their health.
The challenges are seemingly daunting; everyone is wary of sharing data, cyber-attacks, and other digital catastrophes that make trust hard to come by. But on the other side, digital has a lot to give and creates an incredible amount of value in healthcare.
VR is treating kids with dementia; AI is helping with better and faster drug discovery, technology is helping in unforeseen ways.
But there are privacy concerns, over cybersecurity, and there are ethical concerns as well. To develop a better future for human health, we must collectively resolve and regulate these issues. Also, a positive regulatory perspective will be the key in deciding the pace of digital healthcare. There are a multitude of reasons to cheer for technology; we must embrace it collectively.
We are an IT product development company working with clients as their technology partner. We provide a high velocity engineering team to build products and custom solutions.
We are a digital catalyst and catalyze solution development with our high-velocity agile delivery model and in-depth tech expertise for global organizations.
Our team consists of passionate techno-functional experts that bring an outside-in approach and work as an extension of client teams. We are industry agnostic and work with companies of all sizes including disruptive startups.
Contact Us
End Notes
-
Jacob C, Sanchez-Vazquez A, Ivory C. Understanding Clinicians’ Adoption of Mobile Health Tools: A Qualitative Review of the Most Used Frameworks JMIR Mhealth Uhealth 2020;8(7):e18072
-
Rabah Kamal, Daniel McDermott, Giorlando Ramirez, and Cynthia Cox KFF, How has U.S. spending on healthcare changed over time?
-
Virtual health: A look at the next frontier of care delivery, McKinsey,
-
Prashanth Reddy, Elina Onitskansky, Shubham Singhal, and Sri Velamoor; Why the evolving healthcare services and technology market matters; McKinsey, 2018
-
Patel SY, Mehrotra A, Huskamp HA, Uscher-Pines L, Ganguli I, Barnett ML. Trends in Outpatient Care Delivery and Telemedicine During the COVID-19 Pandemic in the US. JAMA Intern Med. Published online November 16, 2020. doi:10.1001/ jamainternmed.2020.5928
-
Source: McKinsey Virtual Health Provider Survey (Nov. 2019) QX8
-
What the pandemic means for healthcares digital transformation, HBR, 2020
-
Hermes, S., Riasanow, T., Clemons, E.K. et al. The digital transformation of the healthcare industry: exploring the rise of emerging platform ecosystems and their influence on the role of patients. Bus Res 13, 1033–1069 (2020).
-
Black Book™ - Revenue Cycle Management surveys, 2017
-
A report by the Organization for Economic Co-operation and Development (OECD)
-
Jacob C, Sanchez-Vazquez A, Ivory C. Understanding Clinicians’ Adoption of Mobile Health Tools: A Qualitative Review of the Most Used Frameworks JMIR Mhealth Uhealth 2020;8(7):e18072
-
Dahlhamer J, Lucas J, Zelaya, C, et al. Prevalence of Chronic Pain and High-Impact Chronic Pain Among Adults — United States, 2016



